Discover Out of the FHIR Podcast
Out of the FHIR Podcast

25 Episodes
Reverse
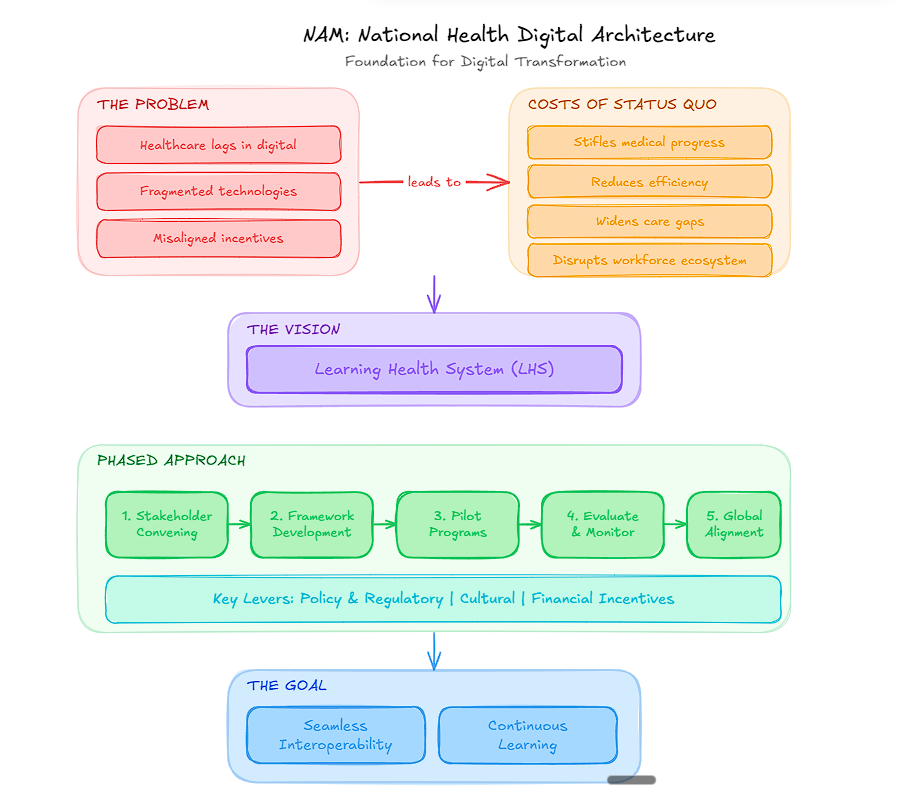
I just got back from HIMSS 2026, and my ears are still ringing mostly from the sound of vendors pivoting to “AI-First” strategies overnight.In Episode 24 of Out of the FHIR, we’re skipping the press releases. I’m breaking down the three biggest lies being told on the conference floor and highlighting the few innovators who are actually using FHIR to move the needle.The “Spicy” Summary:* Stop calling it AI if your data is a mess. Clean FHIR data is the tax you haven’t paid yet.* Interoperability isn’t a tech problem anymore. It’s a “who-gets-paid” problem.* The patient is still an afterthought. Until we stop building silos, “patient-centricity” is just a marketing slogan.Listen to the conversations from the show floor! While at HIMSS I had a chance to look at the National Health Digital Architecture discussion paper released by the National Academy of Medicine.Below are my thoughts on it.The National Academy of Medicine’s (NAM) perspective on a National Health Digital and Data Architecture serves as a direct counterpoint to what is currently unfolding at HIMSS 2026. While NAM proposes a unified, foundational “operating system” for healthcare data, the reality on the conference floor is a fragmented landscape of competing interests.Here is a review of the NAM strategy and why it is not gaining traction in the current HIMSS environment.The Suggested Strategy: A Unified National ArchitectureThe NAM strategy calls for a fundamental shift in how health data is managed:* A Shared Public-Private Utility: Treating data infrastructure as a “common good” (like roads or the power grid) rather than a competitive advantage.* Standardized Semantic Foundation: Moving beyond just “sharing files” to a universal understanding of data meanings (FHIR-native, semantically aligned).* A Single “Architecture of Trust”: A unified framework for identity, consent, and security that removes the need for thousand-point-to-point connections.* Separation of Data from Applications: Storing data in a vendor-neutral layer so that clinical apps can be swapped in and out without data loss.Why This Isn’t Happening at HIMSS 20261. The “FHIR-Washing” of Legacy SilosStrategy: Standardized semantic alignment. Reality: While every booth at HIMSS 2026 prominently displays “FHIR,” most vendors are still “FHIR-washing.” They use FHIR as a thin translation layer on top of their proprietary, legacy databases. This maintains the vendor lock-in that the NAM strategy aims to destroy. True digital transformation requires data to be FHIR-native from the start, but vendors have no financial incentive to rebuild their core architectures.2. The AI Distraction (Infrastructure vs. Shiny Objects)Strategy: Laying the foundation first. Reality: HIMSS 2026 is dominated by Generative AI. Companies are racing to sell the “shiny” end-product (AI clinical scribes, predictive models) while ignoring the “plumbing” (data architecture). AI built on the current fragmented architecture results in “Black Box Silos” AI that only works within one specific EHR or payer system, which is the exact opposite of NAM’s vision for a national learning health system.3. Competitive Moats vs. Common UtilitiesStrategy: Infrastructure as a public-private utility. Reality: In the HIMSS exhibit hall, data is still viewed as an asset to be guarded, not a utility to be shared. The business models of many HIMSS “Anchor Tenants” (large EHR and data aggregators) rely on being the gatekeepers of patient data. There is significant resistance to a national architecture that would commoditize the data layer and force companies to compete solely on the quality of their software applications.4. The “Information Blocking” DanceStrategy: Seamless interoperability by design. Reality: Despite CMS and ONC mandates, “information blocking theater” is in full effect. Companies are technically compliant but operationally obstructive charging high API fees or creating complex workflows that discourage third-party integration. The NAM’s “Architecture of Trust” is impossible to build when the underlying participants are still incentivized to keep data within their own ecosystems.This is why the NAM emphasizes that surface-level technical solutions alone won’t work. You have to resolve the underlying incentive misalignments through policy levers, shared commitment frameworks, and cross-sector collaboration. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In this episode, I sat down with Max Nussbaumer to talk about why he founded Max Health, why he’s bringing his work from Europe into the U.S. market, and what he believes is about to change in healthcare faster than most people realize.Max has deep roots in the FHIR ecosystem from academia at the Technical University of Munich, to Firely, to years of consulting across Europe. Now he’s building something bigger: a company focused not just on FHIR infrastructure, but on how that infrastructure enables real, visible impact for patients through AI, Smart on FHIR, and even wearable integrations.But the real theme of this conversation wasn’t “FHIR adoption.”It was this:Healthcare is about to be reshaped not by standards alone, but by what AI can now do with standardized data.FHIR Is No Longer NicheMax pointed out something many of us have felt over the past year:FHIR used to be a niche standard discussed at connectathons and DevDays.Now it’s the plumbing behind consumer AI health integrations from tools like ChatGPT and Claude.For the first time, health data is entering general-purpose reasoning systems that people use every day. That changes the game. Not because FHIR is new, but because AI can finally use FHIR data at scale.“Software Is Inflationary”One of Max’s best lines:What used to take a year to build can now be built in days.This is showing up at hackathons, startups, and even among 18-year-old builders experimenting with AI, spatial awareness, and real-time health event detection. The barrier to building healthcare software has collapsed if you understand the underlying problems.The differentiator is no longer coding skill.It’s domain understanding and knowing what problem is worth solving.The Real Problem: Incentives, Not TechnologyMax made a powerful comparison:In aerospace, countries cooperate on standards to prevent planes from colliding mid-air.In healthcare, we still don’t have true global data standards because the financial incentives don’t demand it.Healthcare costs continue to rise (approaching a quarter of U.S. GDP), yet most digital tools help people navigate the system, not reduce the need to use it.The real opportunity for AI + FHIR is:* Preventing unnecessary ER visits* Supporting preventative care* Giving patients usable access to their data to power their self care* Enabling decision support before care becomes expensiveWhere AI Changes Healthcare FirstAccording to Max, the most immediate impact won’t be in replacing doctors.It will be in:* Extracting structured FHIR data from unstructured inputs* Real-time scene and event understanding (AI + spatial awareness)* Reducing overload in emergency systems* Supporting remote diagnostics and distributed care models* Turning patient data into actionable, evidence-based guidanceWe’re moving from:“How do we move data between systems?”to“How do we use this data to keep people out of the system?”The Future of FHIR: Less Open, More PreciseWe also discussed the direction of FHIR R6 and the move toward tighter, more stable core resources while allowing innovation to happen in defined spaces.Max’s view: this won’t reduce innovation it will accelerate it. Builders will have more certainty that what they implement won’t shift under them, while AI makes data mapping across standards increasingly trivial.A Global ViewHaving worked across Europe and now the U.S., Max sees strengths and weaknesses in both systems. What’s clear is that:Both systems need better use of data, and patients need more control and transparency.That’s a central theme of Max Health and why he remains deeply committed to open source and global standardization efforts.Where to Find Max* Newsletter: maxhealth.tech* LinkedIn: Max Nussbaumer* Conferences, connectathons, and anywhere FHIR builders gatherThe Big TakeawayThis episode wasn’t about FHIR history.It was about this moment.AI has arrived at the exact time when healthcare finally has a usable data standard. The combination means we can stop talking about interoperability as a goal and start using it as a foundation to solve real problems.And the people who understand both the data and the problems are about to build very quickly. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Top 10 Takeaways: COVID, Data, and the Coming AI Reckoning in Healthcare1) Healthcare didn’t lack data. It lacked urgency.The pandemic didn’t introduce new analytics capabilities. It changed the cost of being slow. When delay becomes lethal, organizations suddenly discover they can make decisions in hours instead of quarters. That tells you something uncomfortable: speed was optional until it wasn’t.2) The winning move wasn’t better dashboards. It was deciding which questions mattered.Pre-COVID analytics chased curiosity. During COVID, analytics chased survival. The shift wasn’t technical sophistication it was ruthless prioritization. Moneyball lesson: when resources are constrained, focus beats breadth every time.3) Interoperability works best when you shrink the problem space.Northwell didn’t unify 70+ EHRs. They built a currently admitted patient index a small, high-value dataset tied directly to decisions. That’s classic systems strategy: optimize the part of the system where leverage is highest.4) Real-time analytics requires trust more than compute.Two daily huddles. Locked pipelines. Tight access controls. The goal wasn’t “more data.” It was shared belief in a small number of metrics. In complex systems, trust is the scarcest input.5) AI turns data quality from a nuisance into a risk multiplier.Bad data used to waste time. Now it produces confident, well-phrased errors at scale. AI doesn’t clean your data it accelerates whatever state your data is already in. This changes the ROI math on governance overnight.6) The most dangerous bias isn’t malicious. It’s missing context.Models assume you’ve provided enough information. Healthcare almost never does. Missing baselines, fragmented history, and unspoken nuance quietly distort outputs. This is the hidden error term no benchmark fully captures.7) Consumer AI creates a parallel healthcare system with no referee.Patients are already using AI for triage, interpretation, and reassurance outside clinical workflows. There’s no visibility, no accountability, and no feedback loop when the model is wrong. That shadow system will shape outcomes whether clinicians like it or not.8) Accountability in healthcare AI is misaligned and unstable.Clinicians and health systems bear liability once AI output enters care. Vendors largely don’t. Patients bear risk when they self-diagnose with consumer tools. That imbalance won’t survive contact with real harm. Regulation is coming but likely late and blunt.9) AI exposes healthcare’s incentive structure, not just its data gaps.If AI reduces unnecessary visits, insurers benefit first. If it increases demand through anxiety, providers feel the strain. Like Moneyball, the advantage won’t come from better tools it will come from understanding who wins and loses under new rules.10) The real competitive advantage isn’t smarter models. It’s judgment.AI can summarize, predict, and suggest. It can’t know what matters most right now. The organizations that win won’t be the ones with the fanciest AI. They’ll be the ones that combine clean data, tight feedback loops, and humans who know when not to trust the machine. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In Episode 21 of Out of the FHIR, I sat down with Pooja Babbrah, Executive Vice President of Strategy and Industry Alignment for NCPDP. We bonded over our shared history in the pharmacy world dating back to the rivalry between Medco and PCS and dug deep into why pharmacy is the sleeping giant of healthcare interoperability.Here are the key takeaways from our conversation:1. Pharmacists Are Care Team Members, Not Just DispensersWe often view pharmacy as a transactional space, but Pooja highlighted the shift toward clinical services. From COVID vaccinations to managing chronic conditions, pharmacists are often the most accessible healthcare providers in rural communities. However, to fully integrate them into the care team, they need access to clinical data (labs, diagnosis) that currently lives trapped in the EHR.2. The “Better Together” Story: NCPDP + FHIRA common question Pooja gets is: “Why don’t we just do everything in FHIR?”. Her answer is crucial for architects to understand:* NCPDP has mastered real-time transactions over the last 40 years (claims adjudication, eligibility). You don’t fix what isn’t broken.* FHIR is the clinical bridge. It allows pharmacists to pull the clinical context needed for prior authorization or care coordination, which can then be wrapped into an NCPDP standard for the payer. It’s not an or; it’s an and.3. The AI & Patient Empowerment FrontierWe discussed the controversial but exciting potential of AI in pharmacy. While headlines panic about “AI refills,” the reality is that basic maintenance meds (like statins) are perfect candidates for auto-refill workflows, provided the pharmacist is looped in to check labs and vitals. Pooja and I both agreed that the “Holy Grail” is an AI agent that acts as a proactive partner scheduling appointments, reconciling meds, and reminding you to pick them up so caregivers aren’t left managing complex logistics alone.4. Interoperability is a Business Problem, Not a Tech ProblemI shared my recent nightmare trying to schedule a colonoscopy stuck in phone queues and filling out 50-question Word documents because the referral data didn’t move. Pooja noted that while the “pipes” (TEFCA, FHIR) are being built, the business incentives to share that data are still lagging.What’s Next? Keep an eye on the NCPDP Collab (a workflow-focused event in February) and the new consumer-facing real-time benefit check pilots. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
This episode of Out of the FHIR features Paulius Mui, MD, a family physician and entrepreneur, exploring the critical intersection of clinical medicine, technology, and data standards. Dr. Mui shares his journey from residency to becoming a tech-savvy clinician and advocate for primary care, discussing the challenges of quality measurement, the evolving healthcare workforce, and how technologies like FHIR and AI scribes are transforming or failing to transform clinical practice.🌶️ Spicy Takes* The Quality Measurement Farce: Gene points out the absurdity of current metrics, like ADHD “management” only requiring two follow-up visits a yeah a bar so low it’s practically meaningless.* The AI Scribe Illusion: A recent study suggests AI scribes don’t actually save physicians time; they just shift the workload from documenting during a visit to reviewing and editing after it.* The NP Training Gap: Dr. Mui highlights the concern over the “boom” in nurse practitioner programs with minimal in-person training compared to the rigorous, repetitive clinical hours required in traditional residency.* “Vibe Coding” vs. Healthcare Reality: While AI-assisted prototyping (vibe coding) is great for front-end ideas, the back-end healthcare infrastructure remains notoriously difficult and rigid.💡 Key Takeaways* Innovation via Proximity: The most effective solutions come from those closest to the problem. Clinicians who understand both medical and technical workflows are best positioned to fix healthcare’s bottlenecks.* Skills-Intelligence for Quality: Healthcare should move away from just “checking boxes” and toward measuring specific competencies (like pattern recognition or antibiotic stewardship) to identify where clinicians need support.* Stop Reinventing the Plumbing: Healthtech startups shouldn’t have to rebuild back-end infrastructure (FHIR connectivity, etc.) from scratch. Standardized “plumbing” allows for faster innovation.* The Power of a “Beginner’s Mind”: Dr. Mui encourages experts to lead with inquiry. Writing and sharing simple questions often leads to deeper insights than trying to maintain an “expert” persona.* Sustainability is the Goal: With healthcare spending nearing a third of the US GDP, technology’s primary role must be to create a sustainable model that actually improves patient experience and clinical outcomes. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
This week, I’m sharing a special conversation I had with Aaron Neiderhiser of Tuva Health and Phil Ballentine from Atropos Health (together they host the High Dimensional Health Data Podcast) . We’ve been trying to schedule this for months, and I’m glad we finally hit record because we got right into the weeds of why healthcare analytics is still so painful and how we are fixing it.If you’ve followed my work, you know I’m obsessed with the intersection of FHIR and Analytics. But there is often a disconnect between the “high priests” of standards and the data engineers trying to run SQL queries in relational databases.In this episode, we bridge that gap.We discuss:* The SQL on FHIR Conference: Why the industry is standardizing “View Definitions” to make FHIR portable across different data warehouses.* CQL vs. SQL: Why Clinical Quality Language is great for requirements, but SQL (aided by AI) is another way to execute at scale.* The “Dump Truck” Theory: Why APIs aren’t always the answer for analytics teams who just want bulk data access.* Automating Interop: How I’m using AI Agents to do the grunt work of mapping and flattening data, so you don’t have to wait on “Larry” (the fictional, overworked hospital IT admin) to run a report for you.It was a blast recording with the High Dimensional team they bring a refreshing, “not just drinking the FHIR Kool-Aid ” reality to the conversation that is often missing from standards discussions.Enjoy the listen!GeneSpicy Takes* The “Windows ME” of Standards: We discussed how the industry seems to be collectively skipping FHIR R5 (like Windows 95/98 to 2000) and waiting for FHIR R6 to become the normative standard, avoiding the “trough of disillusionment” associated with intermediate versions.* The “Larry” Bottleneck: We personified the interoperability problem as “Larry” the overworked IT guy at the health system who smokes two packs a day, takes three lunches, and ignores your ticket for a claims feed. The goal of Bulk FHIR is to bypass the “Larry problem,” but we aren’t quite there yet.* Phil’s Hot Take: In a moment of pure chaos, Phil claimed Windows ME was the best operating system ever made. (We agreed to disagree). Fun Facts & Why You Should Listen* The Portuguese Connection: I shared a story about meeting Grahame Grieve (the “Father of FHIR”) at a FHIR camp in Portugal, highlighting how the “open” nature of the standard was intentional, even if it creates headaches for data modelers today.* Real-Time Solutions: We discuss actual tools (like the Tuva Project and Health Samurai) that are solving these problems now, not just theoretically.* Why Listen: If you have ever stared at a nested JSON object and wondered how to get it into a dashboard without crying, this episode explains exactly how the industry is solving that problem. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In today’s rapidly evolving healthcare landscape, the integration of data between payers and providers has become crucial for delivering value-based care. In this episode of the out of the fhir podcast, FHIR Data guy sits down with Michael Westover , VP of Payer Partnerships and Informatics at Providence, to discuss his journey in healthcare, the challenges of data integration, and strategies for successful value-based care.The Journey to Value-Based CareMichael Westover’s path to his current role began with a strong foundation in healthcare consulting, where he guided states and municipalities on healthcare benefits. His desire to be closer to the action led him to pursue an MBA with a healthcare emphasis, eventually joining a startup focused on data integration and analytics. Westover highlights the importance of understanding both the business and clinical sides of healthcare, stating that the business of healthcare differs significantly from patient care.Challenges of Data Integration One of the most pressing issues in healthcare today is the complexity and fragmentation of data systems. Westover describes the cumbersome process of sharing data with vendors, where a simple request for longitudinal data can take months to fulfill due to the vast number of different systems involved. He emphasizes that healthcare organizations often struggle with outdated methods of data exchange, relying on CSV files and manual queries that can lead to errors and inefficiencies.The Importance of StandardizationWestover advocates for standardizing data practices to improve interoperability. He notes that while there are national initiatives like TEFCA aimed at enhancing data exchange, there remains a significant gap in sharing the right data. By collaborating with payer partners to identify crucial data needs, Providence has successfully established strong relationships that benefit both parties. This collaboration allows for more accurate data exchange, which is essential for effective value-based care.Success Stories notable example of successful data integration is Providence’s partnership with Humana. Their collaboration focuses on using national data standards, such as FHIR, to streamline data exchange through standardized APIs. This approach enables both organizations to access and share critical information, such as member rosters and clinical data, efficiently. Westover explains that aligning incentives and fostering open communication have been key to this success, as both parties recognize the importance of accurate data in achieving high-quality patient care.Key Takeaways: Westover’s insights shed light on the vital role of data integration in advancing value-based care. Key takeaways include:1. The journey to effective data integration requires a deep understanding of both clinical and business aspects of healthcare.2. Standardizing data practices is essential for overcoming the challenges of fragmentation and inefficiency.3. Building strong partnerships with payers can lead to improved data exchange and better patient outcomes.4. Successful collaborations, like that between Providence and Humana, demonstrate the power of aligning incentives and fostering open communication.As the healthcare industry continues to adapt to value-based care models, the importance of effective data integration cannot be overstated. By learning from successful partnerships and advocating for standardized data practices, healthcare organizations can work together to improve patient outcomes and streamline operations. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Welcome back to Out of the FHIR. This isn’t just any episode. This is a reunion.FHIR Data guy brings together two heavy-hitters from his past, Eric Melymuk Principal Engineer at Progyny and John Dobak Senior FHIR Analytics Engineer at b.Well a trio of veterans who all came up in the “bad old days” of HEDIS and traditional quality measurement.This is the story of a technology stack (and a mindset) that defined healthcare data for decades, and the new stack that’s poised to replace it. They dive deep into the messy, complicated, and fascinating transition from the world of custom SQL, claims data, and regulatory checklists to the new frontier of FHIR, CQL, and true clinical interoperability.Hot Takes* The “Mind Shift” Thesis: Perfectly stated by Eric, is that the move from traditional SQL-based reporting to FHIR + CQL (Clinical Quality Language) isn’t just a syntax change. It’s a fundamental mind shift away from “logic customized to my organization” and toward “universal clinical intent.” This is the unlock.* Beware the “Gray Water”: The biggest risk of the new FHIR-based world is creating “dirty FHIR data.” It’s data that is technically compliant (it passes the validator!) but is clinically useless. He calls this “gray water,” and it’s the next great crisis. Organizations treating FHIR as a low-cost, check-the-box “cost center” are just propagating this gray water downstream, poisoning the well for everyone else.* The “Consumer Reports” Blind Spot: For decades, HEDIS and Star Ratings have been the “Consumer Reports for healthcare” (John’s analogy). The problem? We’ve been hiding the magazine from the consumers. The real promise of FHIR isn’t just better back-end reporting; it’s finally putting that quality data into the hands of the patients making the decisions.* LLMs as the Co-pilot, Not the Pilot: ”Do we even need measures in the age of AI?” Yes. But AI and LLMs aren’t the replacement for clinicians or measures. They are the co-pilot (Eric’s term) that helps builders create the logic and test cases, and they may become the translator that finally makes this data understandable to a patient.* The Cultural Battle: This isn’t a technology problem; it’s a culture problem. The entire panel agrees: if your organization views FHIR and interoperability as a regulatory “cost center,” you’ve already lost. The winners will be the ones who find executive champions (Eric’s point) who understand this is a new product and the strategic foundation for everything that comes next.From Brittle SQL to a FHIR FutureThis conversation is a journey from the past to the future of healthcare data.Act 1: The Old World (The HEDIS Grind) The guys reminisce about the “hardest problem” in health tech: traditional quality reporting. It was a world of brittle, custom-built SQL engines, siloed (and non-technical) quality departments, and a total dependency on claims data not because it was the best data, but because it was the only consistent data.Act 2: The New Stack (The FHIR/CQL Unlock) Gene pivots the conversation to the “new stack.” The difference is night and day.* Old Way: NCQA hands you a 200-page book (Volume 2) and says, “Good luck.” You have to design the schema, the logic, the whole thing.* New Way: NCQA hands you the code. The schema is the FHIR Implementation Guide (IG). The logic is the executable CQL file. The entire low-level, error-prone interpretation is abstracted away.Act 3: The Messy Middle (The “Gray Water” Problem) But this transition is where the real drama is. The panel identifies two massive risks:* The Data Itself: We’re moving from clean claims data to messy, unstructured clinical (EHR) data. The old logic (built on claims “artifacts” like Place of Service codes) simply doesn’t map.* The “Cost Center” Trap: Because of regulatory mandates, organizations are scrambling to create FHIR data. They’re doing it cheap, fast, and without clinical governance. This creates John’s “gray water”FHIR bundles that are valid but meaningless, which will break everything downstream.Act 4: The Real Goal The episode concludes by refocusing on the why. Eric makes the passionate case that we’ve “lost sight” of the goal. It’s not about checking boxes for payment; it’s about improving care. The new stack (FHIR, CQL) is the first real chance to build systems that give data back to providers and patients in real-time, finally fulfilling the original promise of quality measurement.The Playbook: Learnings from the HEDIS OGs* 1. Don’t Replace the Warehouse, Feed It. This is a key strategic insight from John. CQL and FHIR do not replace your SQL data warehouse. They work together. Use the CQL engine to process the messy, real-time FHIR data, and then use the output (the FHIR MeasureReport resources) to feed your traditional SQL warehouse for population-level analytics. It’s the best of both worlds.2. Your FHIR Implementation Is Your Product. The panel’s biggest warning: do not treat your FHIR implementation as a “cost center” or an IT project. It is a product. It requires governance, clinical input, and executive champions. If you don’t, you’ll spend millions building a “dirty data” engine that provides no value.* 3. Use the EOB as Your Bridge. How do you get from a claims-based world to a clinical-data world? Eric points to the bridge: the ExplanationOfBenefit (EOB) FHIR resource. It’s designed to model adjudicated claims. This allows you to “dip your toe in” by mapping your existing, clean claims data into a FHIR structure first, before you tackle the mess of raw EHR data.4. Get Your Feet Dirty (The Community is Open). The single best way to learn is to do. The HL7 FHIR community (on Zulip) is famously open. As John notes, you can even feed an entire Implementation Guide into an LLM and start asking it questions. The barrier to entry has never been lower. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In this episode, I speak with Mark Scrimshire, Chief Interoperability Officer at Onyx, about his extensive journey in healthcare interoperability, the evolution of data sharing standards, and the future impact of regulations and technology.Mark Scrimshire’s Journey to FHIR®Mark recounts his two-decade career, which provides a vivid history of modern interoperability. His journey began around 2009 during the American Recovery Act, where early initiatives like CMS’s “Blue Button 1.0” allowed patients to download their claims history—often as a massive, unusable text file thousands of pages long.His pivotal moment came as an Entrepreneur in Residence at CMS, where he was tasked with building a modern API for Medicare beneficiaries. Instead of creating a proprietary standard, he chose to adopt the emerging HL7® FHIR® standard. This project evolved into Blue Button 2.0, a landmark API that proved the viability of using FHIR® at a national scale. He was instrumental in defining key resources like the Explanation of Benefit..This work at CMS laid the groundwork for the 2020 CMS Interoperability and Patient Access final rule, which mandated that payers provide patient access via FHIR® APIs. Seeing this regulatory shift coming, Mark co-founded Onyx to build a platform that helps healthcare organizations comply with these rules and leverage the new data-sharing paradigm.The Power of Regulation as a CatalystA central theme of the conversation is the role of government regulation in driving change. Mark argues that mandates are essential for overcoming industry inertia. He uses the upcoming Prior Authorization rule as a key example. While the rule only mandates the API for certain government-funded plans, he predicts that the efficiency gains (getting an answer in 15 seconds via an API versus days via fax) will create immense market pressure for payers to offer the same capability for their commercial plans. This transforms a compliance requirement into a strategic business transformation.Interesting Observations* Flipping the Script on Data Integration: Mark powerfully articulates a common problem in healthcare IT: an “80/20 rule” where organizations spend 80% of their effort just trying to get the data and only 20% actually using it for analysis and insight. He argues that standardized FHIR® APIs and trust frameworks are designed to “flip this script,” allowing organizations to spend only 20% of their effort on connectivity and 80% on creating value from the data.* The Core Challenge is Trust, Not Technology: Mark asserts that the biggest barrier to seamless interoperability is not a lack of technology but a lack of scalable trust. Establishing individual connections between thousands of payers and providers is a manual, time-consuming process that costs “man-years” of effort. The solution lies in building robust trust frameworks (like TEFCA or security protocols like UDAP) where an entity can be vetted once and then securely connect with anyone else in the network, dramatically reducing friction.* Regulation as a “Bridgehead” for Market Transformation: Mark views regulations not as the end goal but as a “bridgehead” a starting point that establishes a new technical and business reality. Once the infrastructure (like FHIR® APIs) is in place due to a mandate, the market naturally finds innovative and more efficient ways to use it, pushing adoption far beyond the original scope of the rule.* FHIR® as an Enabler for AI, Not a Relic: Addressing the question of whether AI makes standards obsolete, Mark argues the opposite. He states that having well-structured, standardized data from FHIR® APIs makes AI more efficient, accurate, and less resource-intensive. Without standards, AI models would have to waste immense computational power on parsing unstructured documents (like PDFs) and de-identifying data, a process FHIR® makes unnecessary. Standardized data is the clean, reliable fuel that will power the next generation of healthcare AI. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In our latest episode of Out of the FHIR, I had a refreshingly candid conversation with Scott Rossignol of Farseen Advisors. With over 15 years in the trenches, including a formative period at Epic, Scott brings a dose of reality to the often-hyped world of FHIR and interoperability.We didn’t just talk about standards; we talked about strategy, pitfalls, and the hard-earned lessons from building and deploying real-world healthcare applications. If you’re tired of the buzzwords and want to know what it actually takes to succeed, this episode is your guide.Here are some of the spiciest, most crucial takeaways from our discussion:Hot Take #1: Stop Building for Interop. Build a Product People Want.One of the most powerful points Scott made was a fundamental shift in mindset. Too many companies lead with their integration strategy, believing that connecting to data is the product itself. Scott argues this is backwards.He shared an experience of getting a SMART on FHIR app live in just three days. The secret? It wasn’t just the tech. It was a great product solving a clear problem, with motivated stakeholders who wanted it.As Scott put it, the goal isn’t just to “do interoperability.” The goal is to “build a product that works and pleases your customers, and improves with integration.” Your interoperability strategy should serve your product, not the other way around. If the core product doesn’t provide value on its own, no amount of data integration will save it.Hot Take #2: FHIR is a Tool, Not the Whole Toolbox.For developers diving into health tech, it’s easy to assume FHIR is the one-and-only answer. But as Scott rightly points out, clinical and administrative workflows are far too complex for a single standard to solve everything.The perfect example? Real-time notifications. Scott explained, “If you need event-based pushes, like a notification for a patient admission, you’re not going to get that from a standard FHIR API. You’ll need to look at other standards like HL7v2 ADT feeds.”Until FHIR Subscriptions are universally adopted and supported (which is still a ways off), the decades-old HL7v2 standard remains a critical part of the ecosystem. True interoperability experts know how to build a hybrid system, leveraging the best tool for the job whether it’s a modern FHIR query or a classic, event-driven ADT feed.Hot Take #3: National Networks are Promising, But Don’t Hold Your Breath.Initiatives like TEFCA and the CMS Aligned networks promise a future where data flows freely across a “network of networks.” The vision is powerful, but Scott provides a necessary reality check on the current state.While progress is being made behind the scenes, what’s publicly available is often limited. Scott notes that much of the CMS Aligned network’s visibility has been “just a few press releases so far.” The real work of establishing trust, defining mature use cases, and getting participants to exchange meaningful data is a slow, arduous process.His advice for organizations today? Don’t wait for a national network to solve your problems. Identify your specific data needs and find the most direct path, whether that’s through patient-authorized access, regional HIEs, or direct BAA-gated connections. These networks will become incredibly valuable, but you need a strategy that delivers value in the meantime.* On Implementation Reality: “You could have the perfect application that works flawlessly in a sandbox, but if the health system has a six-month security review process, your timeline is six months. That’s the reality.”* On EHR Vendor Differences: “I love that Epic has a great user experience... I love that Cerner provides great write-back capabilities... I love that Athenahealth has a one-click deployment. The fact that I can’t say all those things about one EHR tells you everything you need to know about the challenges of integration.” Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
In a new episode of the "Out of the FHIR" podcast, host Gene Vestel sits down with Mark Kramer PhD of MITRE, a pioneering force in both artificial intelligence and healthcare interoperability. Mark, an original AI innovator, offers a contrarian and thought-provoking take on the future of healthcare data.Don't miss this episode as they discuss:* The radical idea that human language might replace complex healthcare codes. Could the conversational abilities of large language models make traditional coding systems like SNOMED and CPT obsolete?* A "back to the future" approach to patient care. How can AI-powered conversational interoperability bring back the deep, personalized conversations that have been lost in the current fee-for-service, time-crunched healthcare system?* The slow pace of FHIR adoption and the future of healthcare standards. With FHIR implementation guides languishing, is conversational interoperability the catalyst needed to unlock the true value of healthcare data?Get ready to challenge everything you thought you knew about healthcare interoperability and the role of AI.Podcast Platform LinksSubstackSpotifyApple PodcastsYoutubeMust read articles on Conversational Interoperability and report out from the HL7 Connectathonhttps://www.linkedin.com/pulse/conversational-interoperability-takes-shape-read-out-from-mandel-md-379fchttps://www.linkedin.com/pulse/why-conversational-interoperability-essential-future-mark-kramer-retre Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Guests: Bill Lakenan & Benji Graham – FHIR evangelists & innovators at Bellese Where We’re At* CQL maturity: Finally stable enough to calculate without different engines giving different answers. But DEQM (Data Exchange for Quality Measurement) is still a labyrinth powerful, but too flexible and waiting for industry alignment.* QI Core vs reality: Full QI Core adoption is a fantasy today. The pragmatic move is USCDI+ Quality subsets stop boiling the ocean, start with buckets.* NCQA & CMS pressure: Both are turning the screws. NCQA’s push for FHIR-only HEDIS reporting and CMS’s signals on hospital quality programs mean “claims-only” days are numbered.The Payer/Provider DilemmaLegacy organizations face two doors:* Stand up a FHIR-native system* Slap a FHIR façade on legacy infrastructureThe advice: don’t wait. Off-the-shelf solutions exist, but the hurdle is domain expertise and data quality. Bad data = garbage measures. As Gene put it, we’re “building a new house while still living in the old one” but you still have to start building.Holy Grail Moments AheadTwo tipping points will define the dQM journey:* When digital quality becomes cheaper and easier than today’s bloated admin burden.* When FHIR measures double as care gap alerts in real time. Imagine a doctor getting an instant ping “you’re overdue for a colonoscopy” instead of an end-of-year spreadsheet.And let’s not forget the patient. Today’s care gap lists never reach them. The new paradigm? Agents, APIs, and FHIR empowering patients to close their own gaps.FHIR + AI = Frenemies or Besties?* Bill’s take: AI won’t kill standards it’ll sharpen them. Use LLMs to craft better, transparent measures.* Benji’s take: AI + FHIR are a perfect match. FHIR’s granular, graph-like structure is exactly what agents and LLMs love. The future is FHIR-fueled AI workflows, not black-box medicine.Industry Spice* TEFCA & endpoint discovery: The dream is making FHIR directories “as trivial as Google Maps.” Until then, duplicative tests will keep costing patients pain and payers billions.* Gene’s personal mic drop: waiting two weeks for a CD-ROM of med records in 2025. That’s why interoperability still sucks.Final Notes* Benji is launching a FHIR for Business Analysts course this fall finally, something for the non-technical crowd.* Bill continues running DMV “FHIRside dinners” and teaching internal FHIR courses.* And the trio is hyped for the Pittsburgh Connectathon, where theory meets war stories in real time. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Are you living in a world of broken dashboards and unreliable data pipelines? You're not alone. For too long, data has been treated as a downstream problem, an afterthought to be dealt with by overworked data teams.In this special deep dive, we're joined by Chad Sanderson and Mark Freeman of Gable AI to explore the solution: the Shift Left movement and Data Contracts. We break down how this new paradigm treats data as a first-class product, creating a clear, enforceable agreement between the data engineers who produce the data and the teams who consume it.For our listeners in health tech, this conversation is especially critical. Think of the HL7® FHIR® standard itself as a powerful, industry-wide data contract. It defines the precise structure, terminology, and API rules for exchanging healthcare information. Applying a 'Shift Left' mindset means treating FHIR compliance not as a final validation checkpoint, but as a core requirement from the very beginning of the development process. By enforcing the 'contract' of FHIR at the source—before data ever leaves the EHR or clinical system we can build more reliable interoperable systems, reduce costly data errors downstream, and ultimately deliver better value and more effective AI solutions.Tune in to learn:* Why the modern, federated data stack broke our old processes.* How to bridge the gap between software engineering and data teams.* Practical steps to start implementing a "data as a product" culture that delivers real value to your clients.Learn More: Our guests literally wrote the book on this! Check out Chad Sanderson's new O'Reilly book, "Data Contracts," for the complete guide. ADDITIONAL Reading* Gable AI – Data Contracts: Data Contracts Book (Chad Sanderson & Mark Freeman)* Shift Left Data Manifesto: Shift Left* HL7 FHIR Overview: HL7.org FHIR Overview* FHIR Contract Resource: FHIR Contract Definition* FHIR Profiles / StructureDefinition: FHIR Profiling GuideTechnical Tools* HL7 FHIR Validator: FHIR Validator CLI* Gable Data Contract Examples: Example Contract Specs* FHIR JSON Schema (useful bridge): FHIR JSON SchemaAI + Healthcare Context* NCQA Digital Quality Ecosystem: NCQA Digital Measurement* SMART on FHIR: SMART Health ITFHIR Contracts App* 🔧 FHIR Data Contract Generator (beta): appA playground to generate FHIR-based data contracts aligned with shift-left methodology. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Get ready to geek out! This week on "Out of the FHIR," Gene Vestel sits down with the brilliant Kerry Weinberg, co-founder of Phenomenal and a true expert in the trenches of healthcare data and AI.Kerry and Gene jump right into the big questions: Can an AI really understand healthcare without deep medical knowledge? They explore the wild, unpredictable nature of human health data (it's not your average software log!) and Kerry shares a killer story from her time at Amgen about why context is EVERYTHING when building predictive models.The conversation then tackles the big one: AI agents giving medical advice. From today's clinician-in-the-loop systems to the future of patient-facing bots, they discuss the promises, the perils, and the fact that the AI genie is already out of the bottle.Plus, get the inside scoop on the buzzworthy Model Context Protocol (MCP). Is it the next big thing or just a lot of hype? Kerry breaks down the good, the bad, and the tricky parts of getting AI to speak fluent FHIR without making stuff up. This isn't just a tech talk it's a fun, inspiring, and refreshingly real conversation about the passion, purpose, and incredible people building the future of healthcare.Tune in for:* A masterclass on the nuances of AI in health.* The real story behind starting a health-tech company.* An optimistic look at the vibrant and growing FHIR community.* ...and maybe even plans for a future live-coding session on Twitch! Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Welcome back to another episode of Out of the Fire Podcast, where we tackle the hottest topics at the intersection of healthcare, FHIR, interoperability, and technology.This week, I am thrilled to be joined by a true visionary and expert in the health-tech space, Jill DeGraff. If you follow the conversation around healthcare data and policy, you've undoubtedly come across Jill's insightful analysis and forward-thinking perspectives.In this episode, we jump straight into the topic that's lighting up every health-tech feed: the new CMS Interoperability Framework. Just days after its announcement at the White House, Jill helps us cut through the noise and understand what this "moral commitment" from industry leaders and the government truly means for the future of healthcare data.Is this just another initiative, or is it the start of a genuine "race to the top"?In our conversation, we cover:* The 'Why' Behind the New Framework: Jill explains the crisis-level urgency driving this initiative, from the national disease burden to the economic unsustainability of Medicare.* What's Different This Time? We discuss why this framework is more than just "TEFCA 2.0," focusing on its shift from slow, consensus-based iteration to a model of rapid execution and accountability.* "Kill the Clipboard" and Beyond: A breakdown of the key pledges, including the National Healthcare Directory, modern digital identity verification, and the push for a truly seamless patient experience.* Leaders vs. Laggards: Jill offers a compelling analysis of the business implications, arguing that organizations that have invested in modern architecture will thrive, while those reliant on legacy systems will face significant challenges.* Career Insights: We kick off the episode with a fascinating look at Jill's career path from law to health-tech, and she shares invaluable advice for anyone considering a career in consulting."This is a moral commitment... It's about unleashing the creative energy of the private sector to do what it does best, which is innovate and build value for people." - Jill DeGraffThis isn't just a policy discussion; it's a look at the seismic shift happening right now in our industry. Whether you're a developer, a clinician, a policy wonk, or an executive, this conversation provides a crucial map to navigate the new landscape of healthcare interoperability.Listen now to get the full story! Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Welcome to Episode 9 of Out of the Fhir! This week, we're joined by a special guest, Eyal Dviri, Head of the Data Innovation team at Clalit Health Services the second-largest integrated payer-provider organization in the world.In this fascinating conversation, we travel to Israel to explore its unique and rapidly evolving healthcare ecosystem. With a new law mandating nationwide, FHIR-based data portability, Israel is at the forefront of a healthcare data revolution. Eyal provides an unparalleled, on-the-ground perspective on this monumental undertaking, discussing the real-world challenges and strategic decisions involved in modernizing an entire nation's health data infrastructure.Tune in to learn about:* The Clalit Scale: The immense scope of managing data for 14 hospitals and a massive community network within Israel's public health system.* A National FHIR Mandate: How a new law is compelling the entire country to rebuild its data foundation on FHIR, moving from legacy systems to real-time, structured data exchange.* The AI Race vs. Data Foundations: Eyal breaks down the critical tension between the rush to deploy AI solutions and the essential, foundational work of ensuring data quality and interoperability through standards like FHIR.* A Unique Patient Consent Model: A deep dive into Israel's planned Patient Consent Manager (PCM) and why putting the patient in control of their data is a non-negotiable cornerstone of their new ecosystem.* Global Lessons in Interoperability: How Israel's journey offers powerful insights for healthcare systems worldwide, including the US and its TEFCA initiative, on what it truly takes to build a connected health network.This is a must-listen episode for anyone interested in health data interoperability at scale, the practical realities of implementing FHIR, and the crucial relationship between structured data and the future of trustworthy healthcare AI. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
🎙️ Episode 8 – Why Provider Data Is Still Broken (And How to Fix It) | Guest: Ron UrwongseIn this episode of Out of the FHIR, Gene sits down with Ron Urwongse founder of Defacto Health, a self professed Provider Data Nerd, health tech strategist, and one of the sharpest minds in provider data infrastructure to unpack why provider data remains stubbornly inaccurate, fragmented, and operationally painful across the healthcare ecosystem.💡 Ron exposes the root problem: most healthcare APIs are still glorified databases with business logic missing from the stack. He explains how data accuracy isn’t just about syncing directories it's about rebuilding the underlying operational model with intention, alignment, and contextual relevance.🔎 Featured Topics:* Why provider data is only 50% accurate and why that state hasn’t changed in a decade* The myth of a universal provider directory and why a national directory won’t solve what’s fundamentally a business logic problem* How plans, vendors, and digital health players are stuck pushing CSVs and duct-taping endpoints* What it would take to build an AI-native, agent-based model for provider data stewardship* The limits of FHIR and the opportunity to use it as an orchestration layer, not just a data exchange format💥 Key Quote:"You can’t clean up provider data until you change the incentives, rebuild the system logic, and stop pretending it’s just a data formatting issue."This episode is a must-listen for anyone touching provider directories, network management, quality measurement, prior auth, or digital health operations. Ron doesn’t hold back and it’s the perspective the industry needs to hear.🎧 Listen now and rethink what it really means to fix provider data. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
Out of the FHIR – Special Edition: Plaid for Healthcare, Part 2 Episode Title: The Infrastructure Awakens: From Interop Dreams to Data-Driven RealityIn Part 2 of our special double-header episode, Eugene Vestel dives even deeper into the bold vision of a connected healthcare ecosystem with two of the industry's sharpest minds:* 🧠 Brendan Keeler – Interoperability Practice Lead at HTD Health* 🚀 Jason Kulatunga – Founder of Fasten Health, Techstars NYC '24We go beyond the buzzwords and into the infrastructure truths that will define the next decade of healthcare:🔹 Why the FHIR movement is both essential and already obsolete in some ways 🔹 The brutal reality of building consumer-first health tech in a system that wasn't designed for it 🔹 How we might look back in 3–5 years and think, "What were we thinking?" 🔹 Lessons from Plaid’s playbook and what not to copy in healthcare 🔹 The emergence of an autonomous data layer that lets AI act without human crutchesThis isn’t hype. It’s the kind of grounded, uncomfortable, and ultimately liberating conversation we need to have if we want to break through the ceiling of digital health and actually build something better.🔥 If Part 1 sparked the idea, Part 2 sets it on fire. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
🎙️ Out of the FHIR: Deep Dive – Plaid in Healthcare with Brendan Keeler & Jason Kulatunga - Part 1In this episode of Out of the FHIR, we go deep into the future of healthcare interoperability with two visionaries at the forefront of change: Brendan Keeler, Interoperability Practice Lead at HTD Health, and Jason Kulatunga, Founder of Fasten Health and Techstars NYC alum.We explore:* 🧩 What a "Plaid for Healthcare" could really look like* 🔄 Why control, transparency, and patient-directed access are non-negotiable* ⚙️ The architectural and cultural hurdles standing in the way* 📊 How Fasten Health is creating a personal health API layer that empowers individuals with their own data* 🔮 Where we're headed next and what needs to happen to get thereThis conversation is a raw, practical, and energizing look at what it means to rebuild trust and functionality into the healthcare data experience.Whether you're a product leader, developer, or policy wonk, this episode unpacks the real implications of a truly open health data ecosystem and what it’ll take to get us there.Listen now, and join the movement. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe
🎙️ Out of the FHIR Podcast: Part 2 with Joshua Kelly – Highlights🚀 What’s Joshua Excited About?* Payer-to-Payer ExchangeA pivotal shift enabling payers to consume data—not just expose APIs—transforming how charts are transferred and reducing manual burden. Huge potential impact on chart chase inefficiencies and member onboarding.* FHIR-Specific AI Model Evaluations (FIRE Evals)Joshua outlines Flexpa's work on evaluating LLMs for FHIR tasks like:* Extracting structured data from FHIR resources* Generating FHIR bundles from text* Using reinforcement learning with verified rewards (not RLHF) to improve smaller, private models that outperform general LLMs in FHIR use cases* FHIR validate operation as a reward signal in reinforcement learning, opening the door for better automated resource generation.💡 Underrated Innovations* Smart Health Cards & LinksJoshua sees these as massively underutilized. He envisions paper-based lab results with QR codes enabling seamless data transport—a simple but transformative workflow for patients and providers.* Patient “Sneaker Net” as an Interop HackPatients as the natural transport layer—bringing their own data (e.g., via QR codes or printed links) could rival national HIE efforts in utility.* ChatGPT for Patient InsightReal-world use: Eugene shares how he used GPT to interpret his child’s lab results. This is already happening—users are moving ahead of systems.🏦 Financial Interop Lessons for Healthcare* OAuth SuccessHealthcare learned from fintech, starting with OAuth, unlike fintech’s slow rollout.* Why Plaid’s Model Doesn’t Fully Translate* Fewer, more cohesive accounts in finance (e.g., Amex, Chase)* Healthcare data is fragmented across insurers, providers, labs, often with confusing branding (e.g., the "Blue Cross problem")* The Real Challenge? Data Locator ConfusionEven insiders can’t always identify where data lives. This limits the utility of personal health apps or wallets—too niche for mass adoption.🔧 Tech That Needs More Love* SQL-on-FHIRJoshua ranks this as his #2 underrated tech (after Smart Health Cards). While not truly “SQL,” it simplifies FHIR's nested structures into tabular formats—crucial when working with bulk FHIR data.* Flexpa’s Open Resourceshttps://my.flexpa.com* : Free tool to access your health plan data* Flexpa's Payer Directory: Public directory of payer APIs, location access endpoints, etc.🔚 Final Thoughts* The promise of interoperability is not just connectivity—it’s actionable insight, better care, and easier access.* More orgs should share implementation experiences like Flexpa does to reduce duplication across the FHIR ecosystem. Get full access to FHIR IQ playbook at evestel.substack.com/subscribe