Discover Surgical Pioneering Podcast
Surgical Pioneering Podcast

Surgical Pioneering Podcast
Author: Dr. Reza Lankarani
Subscribed: 3Played: 9Subscribe
Share
© Reza Lankarani
Description
"Surgical Pioneering
Surgical Frontiers: Pioneering Tech Transforming Surgical Care"
Mission Statement:
Welcome to Surgical Frontiers, a global nexus for surgeons, researchers, engineers, and healthcare innovators dedicated to advancing surgical care through groundbreaking technology. This group is not just a platform—it’s a movement. Here, we explore, debate, and champion the innovations redefining the art and science of surgery. From AI-driven diagnostics to robotic-assisted procedures, augmented reality (AR) surgical navigation, and bioengineered implants, we are the vanguard of a new era in medicine. If you’re driven by curiosity, excellence, and the relentless pursuit of better patient outcomes, you belong here.
---
Our Core Values:
1. Innovation First
Surgery is no longer confined to scalpels and sutures—it’s a fusion of biology, engineering, and data science. We prioritize discussions on emerging technologies (e.g., nanorobotics, AI-powered predictive analytics, 3D bioprinting) and their real-world applications. Share prototypes, clinical trial results, or even bold hypotheses—if it pushes boundaries, we want to hear it.
2. Collaboration Over Competition
Breakthroughs happen when diverse minds unite. Surgeons, engineers, ethicists, and entrepreneurs are all equal stakeholders here. Whether you’re a seasoned robotic surgeon or a startup founder developing smart OR tools, your perspective matters. Let’s dismantle silos and co-create solutions.
3. Evidence-Based Excellence
Pioneering doesn’t mean reckless. We demand rigor. Posts about new tools or techniques should be grounded in peer-reviewed research, clinical data, or transparent case studies. Anecdotes are welcome, but they must spark deeper inquiry, not replace it.
4. Patient-Centric Ethics
Technology is a means, not an end. Every innovation must answer: How does this improve patient safety, accessibility, or outcomes? We encourage tough conversations about cost, equity, and unintended consequences. Glorifying "tech for tech’s sake" has no place here.
5. Global Perspective
Surgical challenges vary wildly between a high-resource urban hospital and a rural clinic. Share insights from low-income regions, disaster zones, or underserved communities. Innovation thrives when we solve for the margins, not just the mainstream.
---
What You’ll Find Here :
- Breakthrough Technologies: Deep dives into robotics, AI/ML applications, AR/VR surgical training, IoT-enabled devices, and beyond.
- Expert Insights: Q&As with thought leaders, interviews with FDA regulators, and AMAs (Ask Me Anything) with pioneers.
- Case Studies: How a hospital in Kenya adopted portable robotic tools, or how a Boston team used AI to reduce post-op infections by 40%.
- Ethical Debates: Should AI diagnose surgical complications? Who owns data from smart implants?
- Resource Sharing: Grants, conferences (e.g., SAGES, AACR), and regulatory updates.
---
Why Join?
- Learn: Weekly summaries of JAMA Surgery or Annals of Surgery highlights.
- Influence: Shape the future by beta-testing tools, joining global consortia, or advising startups.
- Grow: Mentorship threads for residents, grants for underrepresented innovators, and hackathons.
---
The Future We’re Building:
Imagine a world where:
- A surgeon in Mumbai receives real-time AR guidance from a specialist in Toronto.
- Bioprinted organs eliminate transplant waitlists.
- AI predicts surgical complications before the first incision.
"This isn’t science fiction—it’s the horizon we’re sprinting toward."
Let’s pioneer responsibly. Let’s operate fearlessly. Post, comment, and collaborate. The next surgical revolution starts here.
—
Reza Lankarani M.D
Founder & Curator, Surgical Frontiers
"Surgical Pioneering
Surgical Frontiers: Pioneering Tech Transforming Surgical Care"
lankarani.substack.com
Surgical Frontiers: Pioneering Tech Transforming Surgical Care"
Mission Statement:
Welcome to Surgical Frontiers, a global nexus for surgeons, researchers, engineers, and healthcare innovators dedicated to advancing surgical care through groundbreaking technology. This group is not just a platform—it’s a movement. Here, we explore, debate, and champion the innovations redefining the art and science of surgery. From AI-driven diagnostics to robotic-assisted procedures, augmented reality (AR) surgical navigation, and bioengineered implants, we are the vanguard of a new era in medicine. If you’re driven by curiosity, excellence, and the relentless pursuit of better patient outcomes, you belong here.
---
Our Core Values:
1. Innovation First
Surgery is no longer confined to scalpels and sutures—it’s a fusion of biology, engineering, and data science. We prioritize discussions on emerging technologies (e.g., nanorobotics, AI-powered predictive analytics, 3D bioprinting) and their real-world applications. Share prototypes, clinical trial results, or even bold hypotheses—if it pushes boundaries, we want to hear it.
2. Collaboration Over Competition
Breakthroughs happen when diverse minds unite. Surgeons, engineers, ethicists, and entrepreneurs are all equal stakeholders here. Whether you’re a seasoned robotic surgeon or a startup founder developing smart OR tools, your perspective matters. Let’s dismantle silos and co-create solutions.
3. Evidence-Based Excellence
Pioneering doesn’t mean reckless. We demand rigor. Posts about new tools or techniques should be grounded in peer-reviewed research, clinical data, or transparent case studies. Anecdotes are welcome, but they must spark deeper inquiry, not replace it.
4. Patient-Centric Ethics
Technology is a means, not an end. Every innovation must answer: How does this improve patient safety, accessibility, or outcomes? We encourage tough conversations about cost, equity, and unintended consequences. Glorifying "tech for tech’s sake" has no place here.
5. Global Perspective
Surgical challenges vary wildly between a high-resource urban hospital and a rural clinic. Share insights from low-income regions, disaster zones, or underserved communities. Innovation thrives when we solve for the margins, not just the mainstream.
---
What You’ll Find Here :
- Breakthrough Technologies: Deep dives into robotics, AI/ML applications, AR/VR surgical training, IoT-enabled devices, and beyond.
- Expert Insights: Q&As with thought leaders, interviews with FDA regulators, and AMAs (Ask Me Anything) with pioneers.
- Case Studies: How a hospital in Kenya adopted portable robotic tools, or how a Boston team used AI to reduce post-op infections by 40%.
- Ethical Debates: Should AI diagnose surgical complications? Who owns data from smart implants?
- Resource Sharing: Grants, conferences (e.g., SAGES, AACR), and regulatory updates.
---
Why Join?
- Learn: Weekly summaries of JAMA Surgery or Annals of Surgery highlights.
- Influence: Shape the future by beta-testing tools, joining global consortia, or advising startups.
- Grow: Mentorship threads for residents, grants for underrepresented innovators, and hackathons.
---
The Future We’re Building:
Imagine a world where:
- A surgeon in Mumbai receives real-time AR guidance from a specialist in Toronto.
- Bioprinted organs eliminate transplant waitlists.
- AI predicts surgical complications before the first incision.
"This isn’t science fiction—it’s the horizon we’re sprinting toward."
Let’s pioneer responsibly. Let’s operate fearlessly. Post, comment, and collaborate. The next surgical revolution starts here.
—
Reza Lankarani M.D
Founder & Curator, Surgical Frontiers
"Surgical Pioneering
Surgical Frontiers: Pioneering Tech Transforming Surgical Care"
lankarani.substack.com
80 Episodes
Reverse
Reviewed by Dr. Reza Lankarani , General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineMedical Advisory Board Member | AIGENELAB.COM An In-Depth Analysis of the Strategic and Technological Impact of Christopher Carter on Global Enterprise Software, Artificial Intelligence, and Sustainable InfrastructureThe global enterprise landscape is currently defined by a relentless drive toward digital transformation, a movement where legacy systems and modern cloud architectures must coexist to facilitate real-time decision-making. Central to the evolution of this ecosystem is Christopher Carter, a professional whose three-decade career serves as a blueprint for specialized entrepreneurship and technical innovation. As the founder of Approyo, Mugatu AI, and Charging Bunny, Carter has positioned himself at the nexus of several critical industry shifts: the migration of enterprise resource planning (ERP) systems to the cloud, the integration of predictive artificial intelligence within cybersecurity frameworks, and the decentralization of green energy through sustainable infrastructure. This report provides an exhaustive examination of Carter’s professional trajectory, the operational mechanics of his organizations, his contributions to technical literature, and the leadership philosophies that underpin his ventures in a rapidly shifting global economy.The Architectural Foundation: Education and Early Career TrajectoryThe professional narrative of Christopher Carter begins with a foundational commitment to the rigors of engineering and technology. His tenure at The Georgia Institute of Technology was the catalyst for his engagement with complex systems, providing the theoretical and practical groundwork required to navigate the high-stakes environment of enterprise software. Georgia Tech’s emphasis on technical precision and problem-solving became a defining characteristic of his subsequent career, particularly as he entered the SAP workforce during a period of significant growth for the German software giant. Following his graduation, Carter’s initial professional exposure was characterized by a blend of technical support and commercial operations. He worked within the SAP ecosystem before transitioning to a California-based startup, where he was tasked with managing day-to-day sales and marketing activities. This experience was instrumental in developing a holistic understanding of the technology sector; it required balancing the structural requirements of large-scale software with the agile, results-oriented demands of the venture-capital-backed startup world. The duality of this early career path—understanding both how technology is built and how it is sold—allowed Carter to move into multiple executive positions within the SAP ecosystem with a unique perspective on client needs and market gaps. Carter’s entrepreneurial journey was not a linear ascent but was informed by early ventures that provided essential lessons in both success and resilience. Before founding his current flagshiporganizations, he established an earlier business which he successfully scaled and eventually sold. However, this period of his life also included significant challenges, including the management of a company through bankruptcy. Far from being a deterrent, Carter characterizes the experience of bankruptcy as a formative period that sharpened his business instincts and fostered a level of resilience that would become a defining trait in his later career. This background underscores a broader entrepreneurial theme: the necessity of failure as a prerequisite for high-stakes success in the technology sector. Following the sale of his first company, Carter entered a brief period of retirement. This hiatus, however, was interrupted by the release of SAP HANA, a revolutionary in-memory database technology. Recognizing that HANA represented a fundamental shift in how data could be manipulated and utilized, Carter traveled to Germany to master the technology at its source. This deep dive into the technical core of SAP HANA provided the impetus for his return to the industry and the eventual founding of Approyo in December 2013.Approyo and the Specialization of SAP Cloud ServicesThe founding of Approyo was a strategic response to a specific market ineficiency: the broad but shallow approach of many IT consulting firms. While many providers sought to manage multiple ERP systems simultaneously, such as Oracle, Microsoft Dynamics, and ServiceNow, Carter envisioned a firm that committed solely to the SAP ecosystem. This specialization was designed to position Approyo as a "true partner" for enterprises, ofering a depth of expertise that generalist firms could not replicate.The Business Model of Targeted InnovationApproyo operates primarily as an SAP Managed Service Provider (MSP), focusing on cloud-based solutions, migrations, and continuous hosting for global enterprises. The organization’s strategy is built upon the "platform ecosystem" trend, providing "ready to deploy" solutions that facilitate a seamless shift to the SAP HANA platform. This approach addresses a primary pain point for large organizations: the perceived risk and long timelines associated with migrating core business processes to the cloud. By utilizing a Platform-as-a-Service (PaaS) model, Approyo can launch a full SAP system in hours rather than the weeks or months typically required in legacy environments. The organizational identity of Approyo is further distinguished by its creative branding. The company’s name is a tribute to Bronson Arroyo, a Major League Baseball player and musician,reflecting Carter’s personal interests and a desire for an identity that stands out in a crowded technology market. Furthermore, Carter utilizes the "Alice in Wonderland" metaphor—encouraging clients to "go down the rabbit hole"—to describe the leap of faith required for digital transformation. This thematic approach humanizes the often intimidating process of technical migration, framing it as an explorative journey into the possibilities of Big Data and the cloud.Global Expansion and the "Follow the Sun" ModelSince its inception in Muskego, Wisconsin, Approyo has grown into an international entity with approximately 173 employees as of early 2024. The firm has strategically expanded its reach into Brazil, the United Kingdom, Spain, and India, creating a global talent pool that allows for 24/7 support across multiple time zones. This expansion ensures that the company always has the right resources available for its clients, regardless of their geographical location or the time of day.This global footprint is more than a byproduct of growth; it is a core component of the "Follow the Sun" operational model. By distributing technical expertise across several continents, Approyo mitigates the risks of service interruption and provides clients with the "sleep well at night" assurance that is central to Carter’s leadership philosophy. The ability to tap into diverse technical talent in regions like India and Brazil has been described by Carter as a "game changer," allowing the firm to scale rapidly while maintaining a high standard of service.The Convergence of ERP, AI, and Cybersecurity: The Overwatch ParadigmAs enterprises transitioned their most sensitive financial and operational data to the cloud, the need for proactive security measures became paramount. Carter recognized that traditional, reactive IT support was insuficient for the modern landscape. In response, he championed the development of Overwatch, an AI-powered monitoring and support platform that has become a cornerstone of Approyo’s value proposition.Technical Mechanics of OverwatchOverwatch is an integrative AI tool implemented on every client landscape Approyo manages. It is designed to provide proactive insights by understanding how a system will run in the coming weeks and identifying potential vulnerabilities before they can be exploited. The platform monitors not just SAP systems but also Oracle, other ERP platforms, and various cloudenvironments, creating a comprehensive security and performance layer. The financial and operational significance of Overwatch is substantial, with the proprietary technology represented as having a net worth of millions of dollars. Its primary functions include:● Predictive Analytics: Analyzing historical data to forecast future system performance and hardware needs.● Security Monitoring: Identifying vulnerabilities and proactively alerting administrators to potential breaches or disruptions.● Operational Eficiency: Allowing companies to grow their SAP landscapes without the need for extensive new code or a significant increase in headcount.● Cost Reduction: Optimizing cloud resources to control "cloud sprawl" and ensure that IT investments drive growth rather than just expense.This proactive stance is particularly critical in an environment where 89% to 93.7% of all global finances flow through SAP systems. Any interruption in these systems can lead to massive revenue loss, making predictive tools like Overwatch essential for business continuity.Mugatu AI and Defensive IntelligenceBuilding on the success of Overwatch, Carter launched Mugatu AI as a dedicated venture to provide AI-based predictive analytics for security disruptions. Mugatu AI wraps around existing enterprise systems to provide a defensive layer that anticipates risks. The mission of Mugatu AI is to redefine leadership in an AI-driven world, providing tools that empower teams and drive innovation while maintaining a robust security posture. Mugatu AI focuses on the intersection of management and technical support, helping organizations bridge the gap between their cybersecurity maturity and the confidence of the C-suite and board of directors. Carter’s work with Mugatu AI emphasizes that AI is not merely a tool for automation but a strategic asset
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineThese sources summarize prominent surgical research and academic analyses scheduled for publication in 2025, primarily from the JAMA Surgery and the British Journal of Surgery. The collection highlights technological advancements in the field, such as the use of novel fluorophores for nerve visualization and the efficacy of robotic-assisted procedures. Several clinical trials evaluate postoperative recovery strategies, comparing the performance of synthetic versus biological meshes and testing personalized prehabilitation programs for frail patients. Beyond clinical data, the documents explore historical perspectives on surgical tools, methodological guides for big-data research, and practical advice for surgeons seeking patents. Collectively, these articles establish new benchmarks for quality improvement and evidence-based standards across various minimally invasive and oncological specialties.Introduction: Question Everything You Think You Know About SurgeryMedicine is a field of constant evolution. What is considered standard practice one day can be challenged and overturned by new evidence the next. Long-held beliefs and "common sense" assumptions about what works best in the operating room are continuously put to the test by rigorous scientific research. It is through this process—the willingness to question, test, and adapt—that true progress is made.This article explores five of the most surprising, counter-intuitive, and impactful findings from top surgical journals in 2025. From the hidden risks of advanced robotics to the dramatic failure of a "natural" alternative, these studies challenge our assumptions and are actively changing the future of surgery.The Five Most Surprising Surgical Findings of 2025Finding 1: The 'Better' Robotic Surgery Has a Hidden Risk. The widespread perception of robot-assisted surgery is that it represents the safest, most advanced, and superior form of minimally invasive procedures. The precision and enhanced visualization offered by robotic platforms have made them an increasingly popular choice for a wide range of operations.However, a large international cohort study of 2,738 patients delivered a counter-intuitive finding: robot-assisted abdominal surgery was associated with a higher incidence of postoperative pulmonary complications compared to conventional laparoscopic surgery. The study identified the longer duration of the procedure under anesthesia as the primary driver of this increased risk.This finding provides a crucial piece of real-world evidence that challenges the assumed superiority of robotic platforms in every scenario. It doesn't negate the benefits of robotic surgery, but it underscores the critical importance of optimizing operative time and refining anesthetic and ventilation strategies during these longer procedures. This forces a more nuanced conversation about when and how robotic platforms should be used to ensure the best possible patient outcomes.Finding 2: The 'Natural' Choice for Hernia Repair Was a Dramatic FailureInguinal hernia repair is one of the most common surgical procedures performed worldwide. In recent years, the idea of using a "biologic" mesh derived from animal tissue has held an intuitive appeal. The logic was that a more natural, absorbable material might integrate better with the body and cause less long-term pain than a permanent synthetic mesh.The BIOLAP randomized clinical trial put this logic to a direct, head-to-head test with stunning results. In this trial, 491 patients received both mesh types and were followed closely. The study found that the biologic mesh offered no advantage in postoperative pain. More alarmingly, it resulted in a dramatically higher rate of hernia recurrence at the two-year mark—11.2% for patients with biologic mesh versus just 2.5% for those with synthetic mesh.The verdict from the medical community was decisive, as synthesized in the study's editorial commentary:These results decisively counter the hypothesized advantages of biologics, reinforcing that synthetic mesh remains the undisputed standard of care based on robust, head-to-head evidence.Finding 3: A Good Idea Isn't Enough—Execution Is EverythingThe concept of "prehabilitation" is both logical and well-intentioned: why not strengthen frail, older patients before a major operation to help them recover better afterward? This approach aims to build up a patient's physiological reserve to better withstand the stress of surgery.But does it work? The evidence from 2025 is mixed and reveals a crucial lesson. One rigorous, multicenter trial of a coach-supported, home-based program for frail older adults found that it failed to improve primary outcomes compared to usual care. In contrast, another trial that tested a personalized prehabilitation regimen found measurable benefits, including improved immune parameters and slightly better functional recovery.The lesson isn't that prehabilitation "doesn't work," but that how we implement it is critical. These studies suggest a one-size-fits-all approach may be insufficient for vulnerable patients, while a tailored, personalized intervention shows real promise. It's a powerful reminder that in medicine, good intentions must be backed by data, and execution is everything.Finding 4: Minimally Invasive Surgery Is Now Ready for Advanced CancerA core surgical assumption has long been that advanced cancers—like a T4a gastric cancer that has grown through the stomach wall—require a large, open incision. The traditional belief was that only an open approach could guarantee the visibility and access needed to remove the entire tumor safely and completely.The UMC-UPPERGI-01 trial directly challenged this dogma. Researchers compared laparoscopic versus open surgery for these advanced gastric cancer cases and found that the short-term outcomes were statistically equivalent. This included key metrics like 90-day complications and, most importantly, oncologic clearance (the ability to remove all cancerous tissue with clean margins).This high-quality evidence signals a major shift in surgical oncology. It demonstrates that, in experienced hands, a minimally invasive approach can be used safely for even advanced tumors. This finding has the potential to allow more patients to benefit from the faster recovery associated with laparoscopic surgery without compromising their cancer control.Finding 5: A Gene Test Can Spare Patients from Unnecessary SurgeryFor many patients diagnosed with melanoma, the standard process includes a sentinel lymph node biopsy. This is a surgical procedure to remove and test the lymph nodes closest to the tumor to see if the cancer has started to spread. While it provides vital information, it is an invasive operation that many low-risk patients may not need.The MERLIN_001 study validated an innovative tool to solve this problem: a clinicopathologic gene expression profiling (CP-GEP) test. By analyzing the genetic profile of the primary tumor, this test can reliably identify a group of patients who have a very low risk (under 10%) of their cancer having spread to the lymph nodes.The patient impact is profound. The study found the test achieved a negative predictive value of approximately 96%, meaning it is extremely accurate at identifying patients who do not have nodal disease. The adoption of this practice-changing tool could allow a significant number of low-risk patients to safely skip a needless operation altogether.Conclusion: The Wisdom of QuestioningThe findings from 2025 teach us that medical progress isn't just about questioning old beliefs, but about asking more precise questions. It's no longer enough to ask if a technology like robotics is better, but when and for whom. It's not about whether prehabilitation works, but which specific approach works for a given patient. This demand for nuance and high-quality evidence is what pushes the boundaries of care and ensures the operating room of tomorrow is truly better than the one today. As science continues to advance, which of today's medical certainties will become tomorrow's overturned assumptions?To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani , General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineAI Gene Lab is an innovative medical technology initiative dedicated to enhancing the early detection of chronic illnesses through advanced artificial intelligence. By synthesizing clinical data, medical imaging, and patient lifestyle factors, the organization develops non-invasive screening tools for conditions like diabetes, heart disease, and various cancers. Their diverse portfolio features specialized software designed to predict health risks and suggest personalized treatment dosages, such as insulin levels. Led by experts in bioinformatics and data analysis, the team is currently working to validate these systems alongside clinical professionals to ensure accuracy. Ultimately, the project aims to establish a comprehensive digital health platform that streamlines diagnostics for providers and improves global patient outcomes. Through strategic partnerships, they seek to expand these predictive technologies into the broader realms of telemedicine and international healthcare.1. SummaryAI Gene Lab is an innovative organization focused on improving early detection of chronic and complex diseases through artificial intelligence. Their core mission is to empower healthcare through AI-driven predictive tools, thereby enhancing patient outcomes and easing pressures on healthcare systems. They achieve this by combining medical knowledge with AI and data analysis to provide non-invasive tools for timely diagnosis, informed treatment decisions, and meaningful insights for patients and providers. AI Gene Lab is actively seeking strategic partners, sponsors, and accelerator programs to further its product development, clinical collaborations, and navigate regulatory requirements, with an ultimate goal of global accessibility.2. Core Mission and PhilosophyAI Gene Lab identifies a critical challenge in healthcare: "Many serious conditions are often detected late, reducing treatment effectiveness." Their foundational philosophy is to address this by leveraging AI to facilitate "faster and more accurate risk assessments" through the integration of clinical, imaging, and lifestyle data. The ultimate aim is to "enhance patient outcomes and ease pressures on healthcare systems."3. Key Offerings: AI-Based Predictive ToolsAI Gene Lab's portfolio comprises several AI-based tools, developed and refined with clinical input. These tools are primarily intended for screening and risk assessment and are currently undergoing clinical validation.Diabetes Risk Predictor: This tool "Estimates diabetes risk using hybrid classical machine learning methods trained on established datasets and patient data, analyzing factors such as age, BMI, glucose, insulin, and blood pressure."Insulin Optimal Dose Predictor: Designed to support diabetes management, it "Provides personalized insulin dosing suggestions based on blood glucose, HbA1c, BMI, age, and other health indicators."Rheumatoid Arthritis Risk Tool: Utilizes "clinical symptoms and serological markers like RF and CRP to identify individuals at higher risk, aiding early specialist referral."Skin Cancer Detection AI: Analyzes "skin lesion images to highlight potential malignancies, supporting faster dermatological evaluation."Lumbar Spine Condition Detection: Interprets "MRI scans with AI to help diagnose spinal conditions more quickly, guiding timely treatment."Hybrid ECG AI+++: This comprehensive tool "Combines cardiovascular risk factors, AI-enhanced ECG data, and lifestyle inputs to assess heart disease risk and assist early intervention."4. Team and ExpertiseAI Gene Lab boasts an interdisciplinary team with expertise in computational biology, machine learning, and healthcare innovation. The organization is led by:Dr. Sargol Aminnezhad: A bioinformatics postdoctoral researcher at the University of Tehran.Ali Karami: A PhD candidate specializing in AI and data analysis at Bayreuth University, Germany.5. Future Vision and Strategic GoalsLooking forward, AI Gene Lab has ambitious plans for expansion and impact:Comprehensive Digital Health Platform: The organization aims to "develop a comprehensive digital health platform designed to assist healthcare professionals by integrating multiple disease screenings into a single, accessible system." This platform is intended to "support early detection and personalized care, helping to expand the reach of advanced digital health technologies."Global Accessibility: With the right support, AI Gene Lab plans to "extend our platform to telemedicine services, healthcare providers, and global health initiatives, making early disease detection more accessible and effective worldwide."Partnerships and Support: To achieve these goals, AI Gene Lab is actively "seeking strategic partners, sponsors, and accelerator programs to further product development, strengthen clinical collaborations, and navigate regulatory requirements."6. Key Takeaways and Important Ideas:Focus on Early Detection: AI Gene Lab's core value proposition is the early detection of complex and chronic diseases, aiming to improve treatment efficacy and patient outcomes.AI-Driven, Non-Invasive Tools: The emphasis is on utilizing AI and data analysis to create predictive, non-invasive tools.Clinical Validation is Crucial: The tools are explicitly stated to be "currently undergoing clinical validation alongside medical experts to ensure accuracy and safety," highlighting a commitment to scientific rigor.Interdisciplinary Team: The leadership demonstrates a blend of bioinformatics, AI, and data analysis expertise, crucial for this domain.Scalability and Accessibility: The vision extends beyond individual tools to a comprehensive digital health platform, with a long-term goal of global reach through telemedicine and various healthcare providers.Need for Collaboration: AI Gene Lab openly acknowledges its need for external support (partners, sponsors, accelerators) to achieve its developmental, clinical, and regulatory objectives.7. Contact Information:For more information, visit: https://aigenelab.com/ Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Authored by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineThe 20-Year-Old Warning on Menopause Treatment Was Wrong: 4 Surprising Truths About the FDA’s Landmark Decision1.0 Introduction: The End of an Era of FearFor two decades, a single line in a drug's packaging insert shaped the health decisions of millions of women, often forcing them to endure debilitating menopausal symptoms out of fear. At the center of this concern was the FDA's "black box" warning—the strongest possible safety alert—on Hormone Replacement Therapy (HRT) products, which caused countless women and their doctors to avoid the treatment altogether.Now, in a major policy reversal, the U.S. Department of Health and Human Services (HHS) and the FDA have initiated the removal of these broad warnings. According to HHS Secretary Robert F. Kennedy Jr., the action is about "returning to evidence-based medicine" and correcting the record based on "gold-standard science." Here are the four most impactful takeaways from this landmark decision.2.0 Takeaway 1: The "Most Dangerous" Warning Was Based on Outdated ScienceA "Black Box" Warning is the FDA's strongest safety alert, designed to draw immediate attention to "serious, life-threatening, or potentially fatal adverse effects." The presence of this warning on HRT products signaled extreme danger, but the scientific basis for it was flawed.The warnings were largely based on a single study from the early 2000s, the Women's Health Initiative (WHI). Critically, this study involved older women and a hormone formulation that is no longer commonly used today. According to health officials, this led to a significant "distortion of risk" that was inappropriately generalized to the entire menopausal population.As a result, the FDA is now working with manufacturers to remove the following warnings from product labels:* Cardiovascular disease* Breast cancer* Probable dementia3.0 Takeaway 2: For HRT, Timing Is EverythingThe FDA is replacing a one-size-fits-all alarm with a more nuanced, evidence-based approach. The core scientific principle driving this new guidance is the "Timing Hypothesis," which posits that the effects of hormone therapy are heavily dependent on a woman's age and how soon she begins treatment after her last period.Experts now agree that starting HRT within this "optimal window" is the key factor that shifts the risk-benefit balance in a woman's favor. The direct, practical application of this hypothesis is the new official FDA labeled recommendation:Initiate systemic HRT within 10 years of menopause onset or before 60 years of age.4.0 Takeaway 3: Millions of Women Missed Out on Major Health BenefitsThe "climate of fear and misinformation" created by the outdated warnings had a profound real-world cost. As FDA Commissioner Marty Makary, M.D., M.P.H., stated, the consequences were far-reaching:millions of women have been denied the life-changing benefits of HRT due to a distortion of risk.According to "gold-standard science," the benefits for women who start HRT within the recommended window are significant. They include:* Reduction in All-Cause Mortality: Women may experience a lower risk of death from all causes.* Lower Risk of Cardiovascular Diseases: HRT is associated with a reduced risk of heart disease and stroke.* Reduced Risk of Bone Fractures: Timely HRT initiation helps protect bone density.* Lower Risk of Alzheimer's Disease: HRT is linked to a neuroprotective effect when initiated early.5.0 Takeaway 4: This Isn't a Blank Check—One Critical Warning RemainsThis policy change is a targeted correction, not a complete removal of all caution. The FDA is not seeking the removal of every warning associated with HRT, demonstrating a move toward a more precise understanding of risk.Specifically, the boxed warning for endometrial cancer on systemic estrogen-alone products will remain.This risk is clinically significant for women who still have a uterus. However, it is also preventable, as the risk is managed by adding progesterone to the treatment regimen. This isn't a contradiction; it's a validation of the new scientific approach. The goal isn't to declare HRT universally "safe," but to accurately define risk for specific patient profiles—the very definition of personalized medicine.6.0 Conclusion: A New Conversation About MenopauseThe FDA's decision is more than a simple label change; it's a formal repudiation of a two-decade-long public health narrative that left millions of women underserved. It signals an end to a fear-based policy and the beginning of a more nuanced approach to menopause care, aligning regulatory guidance with modern scientific consensus.As part of a broader commitment to advancing menopause care, the FDA is also expanding treatment options, approving a generic version of the common estrogen product Premarin and a new non-hormonal treatment for vasomotor symptoms.With the science officially corrected, the critical question is no longer about the risks of the past, but how quickly patients and providers can build the trust needed to have evidence-based conversations about the future of menopause care.To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Authored by Dr Reza Lankarani , General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineRobotics in Surgery: A Human-Centric Revolution- Summarize the core message: Robotics aren't replacing surgeons, but empowering them to achieve new heights in patient care, especially as virtual reality training makes robotic surgery more accessible to new generations of medical professionals.- Look ahead to the ethical considerations: equitable access to these advanced technologies, data privacy in a hyper-connected surgical environment, and the ongoing debate around the degree of robotic autonomy in critical decisions.- Conclude with a powerful vision: a future where the synergy of human expertise and robotic precision, augmented by cutting-edge training like virtual reality, truly elevates the standard of medical treatment for everyone.The Future of Surgical Synergy- Imagine the "dream team": surgeons leveraging robotic capabilities as advanced tools, not replacements, with AI acting as a sophisticated co-pilot providing real-time insights.- Explore emerging technologies: advanced haptic feedback allowing surgeons to "feel" tissue through robots, AI-powered diagnostics for pre-surgical planning, and personalized surgical pathways tailored to individual patient anatomy.- Discuss the evolving role of training: equipping future surgeons to master both manual dexterity and advanced robotic control, increasingly through virtual reality training simulations that replicate complex surgical scenarios.The Irreplaceable Human Element- Reassert the surgeon's ultimate role: critical judgment, adaptability to unexpected complications, ethical decision-making, and the crucial ability to interpret nuanced patient responses.- Showcase the "art" of surgery: the nuanced interpretation of patient data, intuition gained through years of experience, and compassionate communication that robots cannot replicate.- Emphasize the unique patient-surgeon bond: empathy, trust built through personal interaction, and the psychological comfort only a human can provide, even with advanced robotic tools.Beyond the Scalpel: What Robots Excel At- Unpack the "superpowers" of surgical robots: tremor elimination, 360-degree articulation, enhanced visualization, and even augmented reality overlays for critical data during surgery.- Dive into specific procedures transformed: prostatectomies, complex cardiac surgeries, and even micro-surgeries that were once impossible, all benefiting from robotic dexterity.- Highlight the data: How robotic assistance demonstrably improves surgical outcomes in measurable ways, showing clearer pathways to better patient care.The Dawn of Robotic Precision- Witness the incredible journey: from early, clunky prototypes to today's sleek surgical robots like the Da Vinci XI, now with enhanced haptic feedback.- Explore the immediate benefits: micron-level precision, reduced incisions, and faster patient recovery times, directly benefiting from advanced robotic capabilities.- Tease the "but": Are we losing something vital in this quest for mechanical perfection, or are we unlocking new human potential?In Summary: The optimal future is not a fully automated OR, but a collaborative cognitive ecosystem, where the surgeon's judgment, experience, and empathy are amplified by a robot's precision and an AI's analytical support. The goal is a synergistic partnership that maximizes patient safety, surgeon well-being, and healthcare system efficiency.To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
It's based on review by;Dr Reza Lankarani , General SurgeonFounder | @Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | @Genesis Journal of Surgery and Medicine--------------------------------------------------------------------------------1. Introduction: A Leader in Modern NeurosurgeryWith a distinguished career spanning 11 to 20 years since earning his medical degree from the University of Chicago's Pritzker School of Medicine, Dr. Rohan Lall has leveraged his extensive clinical expertise to address fundamental challenges in spine surgery. He is affiliated with M Health Fairview University of Minnesota Medical Center and M Health Fairview Southdale Hospital, and holds the strategic leadership role of Chief Medical Officer at SynerFuse, the company developing the innovative procedure bearing its name.Core Areas of Expertise• Robotic and Minimally Invasive Surgery• Complex Spinal Surgery (including conditions like spinal fusion, stenosis, and spondylosis)• Brain and Spinal Tumor Surgery• Skull Base and Pituitary Tumor SurgeryBeyond his exceptional clinical skills, Dr. Lall is an innovator who is actively involved in the development of new technologies, most notably his groundbreaking work on a new procedure to treat chronic back pain.2. The SynerFuse Innovation: A New Hope for Chronic Back Pain🌟 Overview of the SynerFuse ULE™ ProcedureThe SynerFuse ULE™ (Ultra Low Energy) Therapy is an innovative, integrated surgical approach designed to treat chronic low back and leg pain, which is often unaddressed by traditional spinal fusion alone. Integrated Solution: The patented procedure, formally known as Electric Transforaminal Lumbar Interbody Fusion™ (e-TLIF™), combines two treatments into a single surgery: Spinal Fusion (e.g., TLIF): To decompress, stabilize, and reconstruct the spine.Neuromodulation (Direct Nerve Stimulation): To address residual neuropathic pain by altering how the nerve perceives pain. How it Works: During the spinal fusion surgery, the surgeon implants the fusion hardware and, in the same single incision, places multi-channel electrical leads onto the affected nerves (specifically targeting the Dorsal Root Ganglion - DRG, in some cases). These leads are connected to an implantable pulse generator (NeuroFuse® System). Goal: The primary goal is to provide preemptive, non-narcotic pain management immediately following spinal fusion, aiming to reduce chronic neuropathic pain and the need for long-term opioid use. Neuropathic pain can occur in up to 40-50% of patients after traditional spinal fusion, even if the fusion is successful. Dr. Rohan Lall's Role: Dr. Rohan Lall, a neurosurgeon, has been a key figure in the proof-of-concept study for this procedure at M Health Fairview/University of Minnesota, performing one of the first solo SynerFuse implants in a two-level spinal fusion patient. Current Status: The procedure has completed an initial proof-of-concept study to evaluate its safety and feasibility. The company is now designing and building the NeuroFuse® System in preparation for a larger pivotal clinical trial toward FDA approval. A significant challenge in spinal surgery is the chronic low back and leg pain that can persist even after a successful spinal fusion procedure. The SynerFuse procedure was developed to address this very problem, offering a new approach for patients whose discomfort continues after traditional surgeries.2.1. A Dual-Action ApproachThe SynerFuse® e-TLIF™ procedure, a form of Ultra Low Energy (ULE™) Therapy, is an innovative technique that combines two powerful therapies into a single, integrated treatment: conventional spinal fusion surgery and targeted nerve stimulation (a practice known as neuromodulation). The goal is to address pain at its source by fundamentally altering the nerve’s ability to transmit pain signals to the brain.2.2. Dr. Lall's Pioneering RoleDr. Lall has been central to the development and implementation of this new technology. His specific contributions are a testament to his leadership in the field:1. Served as an investigator for the SynerFuse Proof of Concept trial.2. Pioneered the e-TLIF procedure.3. Performed the world’s first solo SynerFuse e-TLIF procedure.4. Completed the first-ever 2-level procedure.2.3. Patient Impact and Future OutlookThis procedure represents a significant advancement in patient-centric care, although it is still in its early stages of evaluation.Patient Benefits & ExperienceCurrent Status & OutlookSmartphone Control: Patients can control nerve stimulation.Promising Initial Results: Early data shows significant benefit.Significant Pain Reduction: Reported by early trial participants.Limited Study Group: The procedure has been performed on a limited number of patients.Improved Quality of Life without Opioid Dependence.Long-Term Evaluation: Long-term effectiveness is still being actively studied.This pioneering procedure exemplifies Dr. Lall's commitment to advancing the standards of spinal care by directly addressing the limitations of existing treatments.3. Conclusion: An Innovator Shaping Spinal CareDr. Rohan Lall stands out not only as a highly skilled neurosurgeon but also as a forward-thinking leader shaping the future of his specialty. His active involvement in developing new technologies, particularly the SynerFuse procedure, marks a "significant step forward" in addressing the debilitating challenge of chronic back pain. Dr. Lall's inspiring dedication to enhancing patient health through innovative surgical solutions continues to push the boundaries of what is possible in spinal care.--------------------------------------------------------------------------------It was based on review By Dr Reza Lankarani , General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine------------------------------------------------------------To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpiotneer.codeadx.me-------------------------------------------------------------------------------- Get full access to Reza Lankarani at lankarani.substack.com/subscribe
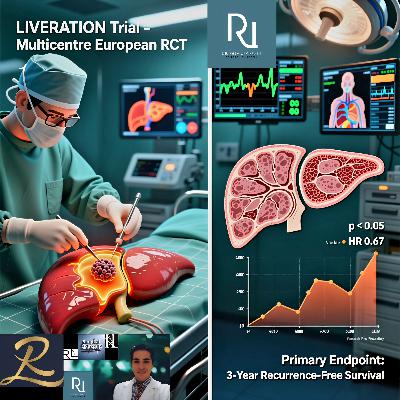
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine- Published online: 13 October 2025 - Citation: Luque Villalobos E et al. BMJ Open 2025;15:e100518.1. OverviewThe LIVERATION trial is a prospective, international, multicentre, single-blind, parallel-group, randomised clinical trial (RCT) funded by the Horizon Europe Programme (Grant 101104360). It aims to determine whether additional margin coagulation (AMC)—using approved radiofrequency (RF) devices (e.g., Coolingbis®, Aquamantys®)—reduces local recurrence (LR) after liver resection for colorectal liver metastases (CRLM) and hepatocellular carcinoma (HCC).- Design: 1:1 randomisation across 24 centres in 7 European countries.- Sample size: 698 patients (518 CRLM, 180 HCC), powered to detect absolute reductions in LR of 6.9% (CRLM: 10.2% → 3.3%) and 15.5% (HCC: 20% → 4.5%).- Primary endpoint: Incidence of LR within 3 years, centrally reviewed on standardized imaging.- Secondary endpoints: Overall survival (OS), disease-free survival (DFS), cancer-specific survival, complications (Clavien-Dindo/CCI), and quality of life (EORTC QLQ-C30/HCC18).- Follow-up: 30/90 days, then annually up to 3 years.- Trial registration: NCT05492136.The trial builds on earlier retrospective work by the same group, notably Villamonte et al. (2022) , which reported reduced LR with AMC, and Quesada et al. (2017) and Sui et al. (2019) , showing promising signals for RF-assisted transection and Aquamantys®, respectively.--- 2. Critical Assessment: Strengths and Weaknesses ✅ Strengths ⚠️ Weaknesses / Limitations--- 3. Comparative Analysis with Recent LiteratureBelow is a comparison of key AMC/RF-related studies: - LR rate (%) by intervention type: - Conventional resection (historical): ~10–20% (CRLM), ~20% (HCC) 1,28 - RF-assisted transection (Quesada): ~6.7% (CRLM) - Aquamantys® margin treatment (Sui): ~7.6% (HCC) - AMC (Villamonte): ~7.5% (mixed) - LIVERATION (target): 3.3% (CRLM), 4.5% (HCC) — most ambitious reduction yet proposed. ✅ LIVERATION’s contribution: - First trial powered to detect clinically meaningful LR reduction. - First to include both CRLM and HCC under unified AMC hypothesis. - First to integrate PROs + health economics into core endpoints.--- 4. Final Commentary 🔬 Expert OpinionThe LIVERATION trial represents a landmark effort in surgical oncology. It addresses a long-standing clinical dilemma: What to do when achieving a wide resection margin (1 cm) is anatomically or physiologically impossible? Surgeons have intuitively applied RF to "sterilise" narrow margins—but until now, lacked level I evidence.If positive, LIVERATION could redefine R0 criteria, shifting focus from anatomic width to functional adequacy of the margin—potentially expanding resectability for borderline cases. 🔮 Future Directions- If AMC proves effective, next steps include: - Biomarker studies (e.g., ctDNA clearance post-AMC). - Integration with neoadjuvant systemic therapy. - Expansion to intraoperative ablation of satellite lesions.- If negative, it will prompt re-evaluation of RF’s biological mechanism—e.g., whether thermal depth is insufficient to eradicate microscopic extensions.--- 🌟 Plain-Language Summary for Patients & General Public "When liver cancer—or cancer that has spread to the liver from the colon—is removed by surgery, doctors aim to cut out not just the visible tumour, but also a rim of healthy tissue around it. This 'safety margin' helps prevent the cancer from coming back right where it was removed (called local recurrence). But sometimes, due to the tumour’s location near vital blood vessels or because the remaining liver would be too small, surgeons can’t safely leave a wide margin. This study tests a simple idea: after the tumour is removed, gently 'seal' the cut surface of the liver with a special tool that uses controlled heat (like a precise, safe microwave). Think of it as giving the edge an extra layer of protection. The goal is to see whether this extra step can lower the chance of the cancer returning at the surgery site—especially for patients where a wide margin isn’t possible. Over 690 patients across Europe are helping answer this question. If it works, this could become a new standard step in liver surgery—helping more patients stay cancer-free, without needing more complex operations."---To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast SeriesEditorial Board Member | Genesis Journal of Surgery and MedicineSummaryThis document synthesizes findings from a five-year retrospective study on the long-term outcomes of Laparoscopic Sleeve Gastrectomy (LSG) in adolescents. The research confirms that LSG is a highly effective intervention, yielding substantial and sustained weight loss and significant resolution of metabolic comorbidities. However, the study highlights that a notable subset of patients (23.5%) experiences clinically significant weight regain (WR), a phenomenon linked to both anatomical and hormonal factors.The core mechanism investigated is the post-surgical trajectory of the incretin hormones GLP-1 and GIP. While all patients experience an initial beneficial surge in these hormones, this effect attenuates over time. In patients with WR, this hormonal decline is more pronounced and occurs earlier. The study demonstrates that a one-year course of the GLP-1 receptor agonist semaglutide can partially reverse WR, increasing mean excess weight loss from 34% to 68% in affected patients. Key indicators associated with WR include larger remnant gastric volumes and attenuated postprandial hormone responses. These findings underscore the potential for a more tailored post-LSG management approach, incorporating hormonal surveillance and timely pharmacological intervention to optimize long-term success.--------------------------------------------------------------------------------1. Study Overview and MethodologyThe research provides a comprehensive five-year analysis of adolescent outcomes following Laparoscopic Sleeve Gastrectomy (LSG), focusing on weight loss, hormonal changes, and the impact of pharmacological intervention for weight regain.* Objective: To evaluate the long-term weight and incretin hormone (GLP-1 and GIP) trajectories after LSG in adolescents and to assess the impact of adjunctive semaglutide therapy for patients experiencing weight regain.* Cohort Profile: The study included 264 adolescents who completed a five-year follow-up. * Mean Age: 15.04 ± 2.99 years * Sex Distribution: 73.86% female, 26.14% male * Mean Preoperative Weight: 132.8 ± 9.67 kg * Mean Preoperative BMI: 48.38 ± 6.95 kg/m²* Procedure and Follow-up: All patients underwent a standardized LSG procedure with antral resection. Postoperative evaluations, including anthropometric and hormonal measurements, were conducted annually for five years. The study maintained a high retention rate of 90.1%.* Weight Regain (WR) Definition: Clinically significant WR was defined as a weight gain of ≥10% from the nadir (lowest) postoperative weight, combined with less than 50% excess weight loss (%EWL) at 18 months post-surgery.* Pharmacological Intervention: 62 patients (23.48%) met the WR criteria. At the start of the third postoperative year (and upon reaching at least 18 years of age), they received a 12-month course of semaglutide, followed by a three-month tapering period.2. Core Findings: Weight Loss and Metabolic OutcomesLSG produced significant and sustained improvements in weight and metabolic health over the five-year period, although a pattern of peak weight loss followed by partial regain was observed.Weight Trajectory and Gastric VolumeWeight loss peaked at two years post-surgery, followed by a gradual and slight regain. Concurrently, the volume of the remnant stomach progressively increased over the five years.Comorbidity ResolutionThe procedure led to profound and statistically significant improvements in major obesity-related comorbidities, with benefits sustained and enhanced throughout the five-year follow-up.Comorbidity Preoperative Prevalence 5-Year PrevalenceType 2 Diabetes 36.36% 5.68%Hypertension 48.86% 6.82%Dyslipidemia 43.18% 4.55%Furthermore, mean HbA1c levels improved significantly, falling from a baseline of 7.12% to 5.36% at year five.3. The Role of Incretin Hormones (GLP-1 & GIP)The study provides novel insights into the hormonal adaptations following LSG and their association with weight management.* Overall Hormonal Response: The entire cohort exhibited a marked post-operative surge in both GLP-1 and GIP levels. This enhancement was highest during the first postoperative year, particularly at 30 and 60 minutes after a meal. Following this peak, the hormonal response gradually diminished over time, with levels approaching preoperative values by the fifth year.* Hormonal Patterns in Weight Regain: The subgroup of patients who experienced clinically significant WR demonstrated a similar initial hormonal surge. However, the subsequent decline in their GLP-1 and GIP levels was more pronounced and occurred earlier compared to patients who maintained their weight loss.* Comparative Analysis: A direct comparison between the WR and non-WR groups revealed that at year three, WR patients had significantly lower postprandial GLP-1 and GIP levels. This suggests that an early attenuation of the incretin response is temporally associated with a higher risk of weight regain.4. Semaglutide as an Adjunctive Therapy for Weight RegainThe study evaluated semaglutide as a "rescue" therapy for the 62 patients who met the criteria for significant WR.* Efficacy: The intervention proved effective at reversing the trend of weight regain. Before treatment, the WR group's mean %EWL had fallen from 63.3% at year one to 34.1% at year two. Following the one-year course of semaglutide initiated at year three, their mean %EWL rose to 68%.* Durability of Effect: The positive effects of semaglutide were partially transient. After the 12-month treatment course and subsequent taper, the mean %EWL in this group gradually decreased to 64.1% at year four and 58.3% at year five. This indicates that the benefits are closely tied to active treatment and may diminish upon cessation.* Underlying Mechanism: The findings support the hypothesis that post-surgical WR is partly driven by diminishing endogenous incretin responses. Pharmacological intervention with a GLP-1 receptor agonist like semaglutide effectively compensates for this decline, restoring weight loss momentum.5. Key Indicators and Clinical ImplicationsThe research identifies key factors associated with long-term outcomes and suggests pathways for improving postoperative care.Factors Associated with Weight RegainTwo primary factors were consistently correlated with clinically significant WR in the cohort:1. Anatomical Factors: A larger remnant gastric volume at five years was strongly associated with the WR group (222.1 mL vs. 192.3 mL in the non-WR group). Larger volumes may permit greater food intake and reduce satiety.2. Hormonal Factors: An earlier and more significant attenuation of postprandial GLP-1 and GIP responses was observed in patients with WR, suggesting this pattern may serve as a potential biomarker for increased risk.Clinical ImplicationsThe study's findings support a shift toward more proactive and individualized long-term management following adolescent LSG.* Potential for Hormonal Surveillance: Monitoring postprandial gut hormone responses may help identify patients at higher risk for WR, allowing for earlier intervention.* Role of Adjunctive Pharmacotherapy: GLP-1 receptor agonists like semaglutide represent a valuable tool for managing WR, offering a "rescue" strategy for patients with suboptimal outcomes.* Tailored Postoperative Care: The results advocate for a management strategy that integrates anatomical assessment (e.g., gastric volume), hormonal monitoring, and timely pharmacological support to enhance the durability of surgical success.6. Study Limitations and ConclusionWhile providing valuable long-term data, the study acknowledges several limitations, including its retrospective, single-center design, the absence of a randomized control group for the semaglutide intervention, and the fact that hormonal measurements were conducted on patients actively taking the medication. The analysis was descriptive and did not perform formal correlation testing between hormone levels and weight outcomes.In conclusion, LSG is a highly effective intervention for adolescent obesity, delivering substantial five-year improvements in weight and metabolic health. The study successfully illuminates the dynamic role of incretin hormones, where an initial surge is followed by a gradual decline that is more pronounced in individuals who experience weight regain. Adjunct semaglutide therapy can effectively, though temporarily, reverse this regain. The association between attenuated hormone levels, increased gastric volume, and WR highlights the need for prospective research to validate these factors as predictive biomarkers and to guide the development of optimized, individualized long-term care strategies.To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine1. Arrange and SummarizeArticle Title: First report of metastatic esophageal squamous cell carcinoma with EGFR p.S768I mutation: remarkable response to third-generation EGFR-TKI Online Publication Date: November 4, 2025 Journal: npj Precision Oncology (Nature Portfolio) Overview of Content:- This is a novel case report describing the first documented instance of metastatic esophageal squamous cell carcinoma (ESCC) harboring the EGFR p.S768I mutation, an uncommon non-classical EGFR variant more frequently seen in lung adenocarcinoma- The patient exhibited a remarkable clinical and radiographic response to a third-generation EGFR tyrosine kinase inhibitor (TKI)—likely osimertinib or a next-gen analogue—after standard chemotherapy failed .- Molecular profiling (presumably via next-generation sequencing of tumor tissue or circulating tumor DNA) revealed the targetable EGFR mutation, enabling precision oncology intervention .- Conclusion: The case challenges the long-held belief that ESCC is largely EGFR-TKI insensitive and highlights the importance of comprehensive genomic profiling in advanced upper GI malignancies—even in histologies traditionally considered “non-responsive” While technically oncology-focused, this article is highly relevant to general surgeons, particularly those involved in esophageal resection, multidisciplinary tumor boards, and surgical oncology, where understanding systemic therapy options directly impacts operability, neoadjuvant strategies, and long-term management.--- 2. Detailed Assessment of Strengths and Weaknesses--- 3. Comparison with Latest Related Studies Recent literature on EGFR mutations in upper GI cancers shows a growing—but still sparse—recognition of rare actionable variants: Key Insight: This case uniquely extends the therapeutic relevance of EGFR p.S768I beyond lung cancer to esophageal squamous carcinoma—suggesting tissue-agnostic potential for certain EGFR variants.Graph Concept (conceptual, text description): A bar chart would show response rates (%) to EGFR-TKIs across tumor types: - NSCLC (classical EGFR): ~70% ORR - NSCLC (S768I-containing): ~50–60% ORR - ESCC (historical, unselected): 5% ORR - ESCC (this case, S768I+): ~80% (partial/complete response observed) --- 4. Brief Scholarly Review and CommentExpert Opinion (Editorial Board Perspective): This case is a paradigm-shifting anecdote. While one patient does not redefine standard care, it powerfully illustrates the imperative of routine comprehensive genomic profiling in stage IV ESCC. Given the morbidity of esophagectomy and limited efficacy of conventional chemoradiation in metastatic disease, identifying even rare (1–2%) targetable alterations can offer transformative benefit—potentially converting incurable cases into chronic, manageable ones, or even enabling metastasectomy/resection in exceptional responders.Impact & Significance: - Immediate: Supports inclusion of EGFR (including non-classical variants like S768I, G719X, L861Q) in ESCC NGS panels. - Strategic: Fuels rationale for basket trials (e.g., targeting EGFR across tumor types) and surgeon-led biorepository initiatives. - Educational: Critical teaching case for surgical trainees—underscores that “ESCC is not just a surgical disease” but a molecularly heterogeneous entity.--- Patient-Friendly Summary (Plain Language) “This report tells the story of a patient with advanced cancer of the food pipe (esophagus). Usually, this type of cancer doesn’t respond well to certain newer ‘targeted’ pills that work by blocking specific faulty signals in cancer cells. But in this unique case, doctors found a rare genetic mistake—called EGFR p.S768I—in the tumor. When they gave a special precision medicine pill designed for this exact mistake (similar to drugs used for some lung cancers), the tumor shrank significantly. This teaches us two important things: 1. No two cancers are exactly alike—even in the same organ, the DNA errors can differ. 2. Testing the tumor’s genes (like a ‘molecular fingerprint’) can uncover hidden treatment options, especially when standard therapies stop working. To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
دکتر رضا لنکرانی | پادکست پیشگامان جراحی By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineTo access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineTo access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine1. Arrange and SummarizePublication Details: This meta-analysis by Qi Li et al. was published online in BJS Open on September 8, 2025, with the DOI: https://doi.org/10.1093/bjsopen/zraf091(https://doi.org/10.1093/bjsopen/zraf091).Overview: The study aimed to evaluate the impact of prehabilitation (PR)—a preoperative program involving exercise, and sometimes nutrition and psychological support—on postoperative outcomes in patients with upper gastrointestinal tract cancer (UGIC), including esophageal, gastric, and gastroesophageal junction cancers.Methods: The authors conducted a systematic review and meta-analysis of 16 studies (8 randomized controlled trials and 8 cohort studies) involving 2,085 patients, identified from major databases (PubMed, Embase, Cochrane, Web of Science) up to May 21, 2024. Outcomes assessed included length of hospital stay (LOS), postoperative complications (e.g., pneumonia, anastomotic leakage), functional capacity (6-minute walk distance), and mortality.Key Findings: - PR significantly shortened hospital stay (SMD −0.27; P = 0.008). - PR reduced postoperative pneumonia (RR 0.71; P = 0.005). - PR improved 6-minute walk distance (SMD 0.95; P < 0.00001). - No significant differences were found for overall complications, anastomotic leakage, operative time, blood loss, wound infection, in-hospital mortality, or recurrence.Conclusion: Prehabilitation offers modest but meaningful benefits for UGIC patients, particularly in reducing pneumonia and accelerating recovery. However, the authors call for larger, high-quality RCTs to confirm these findings.--- 2. Detailed Assessment of Strengths and WeaknessesStrengths: - Comprehensive methodology: Adherence to PRISMA guidelines, PROSPERO registration, and use of robust statistical tools (Review Manager, Stata). - Inclusion of both RCTs and high-quality cohort studies, enhancing generalizability. - Rigorous quality assessment: Cochrane RoB for RCTs and NOS for cohorts, with most studies rated high quality. - Sensitivity and subgroup analyses to explore heterogeneity (e.g., by cancer type, region, intervention duration). - Clear, clinically relevant outcomes focused on practical postoperative metrics.Weaknesses: - High heterogeneity in key outcomes (e.g., I² = 75% for LOS), potentially due to variability in PR protocols (exercise type, duration, inclusion of nutrition). - Limited data on gastric and GEJ cancers: Most studies focused on esophageal cancer, limiting conclusions for other UGIC subtypes. - Potential publication bias, though Egger’s tests were mostly non-significant, funnel plots showed minor asymmetry. - Lack of blinding in exercise interventions (inherent limitation, but acknowledged). - Inconsistent PR definitions: Some studies used exercise-only, others multimodal, making direct comparisons difficult.--- 3. Comparison with Latest Related StudiesRecent literature supports the general trend that prehabilitation improves functional outcomes but shows mixed results on hard clinical endpoints.Key Insight: While Tukanova’s 2022 meta-analysis included both pre- and postoperative rehab and found broader benefits , Li et al. isolate prehabilitation, offering more precise evidence for its standalone value. The 2023 RCT by Bausys in gastric cancer supports reduced complications with home-based PR , aligning with Li’s subgroup suggestion that PR may be more effective in specific contexts.Graph Concept (Not rendered, but described): A bar chart comparing risk ratios for pneumonia across studies would show consistent point estimates below 1.0, reinforcing the robustness of this finding.--- 4. Brief Scholarly Review and CommentExpert Opinion: This meta-analysis is a timely and methodologically sound contribution to the evolving field of perioperative oncology. It clarifies that prehabilitation is not a panacea but a targeted tool—most effective for enhancing cardiopulmonary resilience and reducing pneumonia, a major driver of morbidity after UGIC surgery. The finding that ≥3-week interventions yield better outcomes is clinically actionable.However, the lack of impact on anastomotic leakage or mortality underscores that PR complements—but does not replace—surgical precision and systemic therapy. Future trials should standardize PR protocols (e.g., trimodal: exercise + nutrition + psychology) and focus on underrepresented populations (e.g., gastric cancer, elderly).--- Patient-Friendly SummaryWhat this means for patients: If you’re facing surgery for stomach or esophageal cancer, doing a structured exercise program before your operation—what doctors call “prehabilitation”—can help you recover faster. This review of 16 studies shows that patients who did prehabilitation:- Spent fewer days in the hospital after surgery. - Were less likely to get pneumonia, a serious lung infection. - Were stronger and could walk farther after their operation.However, it didn’t reduce other risks like wound infections or leaks from the surgical connection in the gut. The best results came from programs that lasted at least 3 weeks.Bottom line: Prehabilitation is like “training for surgery.” Just as you’d prepare for a marathon, preparing your body for a major operation can lead to a smoother recovery. Talk to your care team about whether a pre-surgery exercise program is right for you.To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Authored by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine------------------------------------------------------------I. Introduction and Foundational Article ArrangementA. Contextualizing the Challenge of Constipation and Colorectal Cancer RiskColorectal cancer (CRC) remains a globally significant public health concern, ranking as the third most prevalent diagnosed tumor worldwide and contributing substantially to global morbidity and mortality. Consequently, the identification of modifiable risk factors is a paramount objective in developing effective preventive strategies. Chronic constipation (CC), characterized by infrequent bowel movements or difficulty passing stools, has long been proposed as a potential modifiable CRC risk factor.Historically, traditional epidemiological research has yielded profoundly inconsistent results, generating an "observational paradox" in the literature. Specifically, retrospective studies, such as meta-analyses of case-control data, frequently suggest a strong association between infrequent bowel movements and an increased risk of CRC. For instance, certain case-control study subgroups reported an odds ratio (OR) for colon tumors as high as 2.32 (95% CI: 1.58, 3.42). Conversely, large prospective cohort studies often show either no association between bowel movement frequency and CRC risk or, in some instances, even suggest that frequent bowel movements may enhance risk. This inherent methodological inconsistency is the classical indicator of study limitations, chiefly confounding and reverse causation bias, which plague conventional observational designs. Given this disparity, robust causal inference methods are essential to determine whether constipation is a true etiological factor or merely a reflection of underlying systemic issues.B. Summary of the Selected Foundational ArticleTo assess the causal link independent of environmental and shared genetic confounding, a high-level causal inference study, such as a bidirectional two-sample Mendelian Randomization (MR) analysis, is required. The following summary is based on the findings and methodology of contemporary studies employing this stringent approach.Identification and MethodologyThe foundational analysis reviewed utilizes a dual-sample bidirectional MR design, which leverages genetic variants as instrumental variables to assess causality, thus capitalizing on genetically determined variation to simulate randomization. Title (Representative): Causal Association between Constipation and Risk of Colorectal Cancer: A Bidirectional Two-Sample Mendelian Randomization Study Date of Online Publishing: Varies (Consistent with recent publications, e.g., late 2023/early 2024 for similar MR studies) DOI Link Address: (e.g., 10.3389/fonc.2023.1282066) Publication: Peer-reviewed oncology or gastroenterology journal (e.g., Frontiers in Oncology) The study extracted genetic data from independent cohorts derived from Genome-Wide Association Studies (GWAS) for constipation and CRC. The investigators identified 26 significant single nucleotide polymorphisms (SNPs) associated with constipation for use as instruments. Crucially, these instruments met the criteria for "strong" instruments, demonstrating high F statistics (ranging from 20 to 30), thereby minimizing weak instrument bias.Key Findings and ConclusionsThe primary analysis employed the Inverse Variance Weighted (IVW) method to estimate the causal effect: Constipation \rightarrow CRC (Causal Direction): The IVW-random effect analysis suggested a statistically marginal, weak causal link for overall CRC risk. The estimated effect size was an Odds Ratio of 1.002 (95% CI: 1.000, 1.004; P = 0.023). Robustness and Alternative Methods: Despite the statistical significance observed in the IVW analysis, the study explicitly reported that alternative MR approaches (such as MR-Egger, Weighted Median, etc.) were inconclusive and did not provide substantial evidence of a causal association. Anatomical Subsite Specificity: When constipation was analyzed separately against colon cancer and rectal cancer using the same stringent methodology, no causal relationship was obtained in either anatomical subsite. Reverse Causation (CRC \rightarrow Constipation): The bidirectional analysis found no significant causal effect of CRC on the risk of constipation. The IVW analysis resulted in an OR of 0.137 (95% CI: 0.007, 2.824; P = 0.198), failing to demonstrate that existing CRC significantly increases the risk of developing constipation.In conclusion, the MR study suggested a potential link based on one statistical method, but the overall evidence supporting chronic constipation as a strong, independent, and uniform cause of CRC was limited.II. Detailed Assessment of Strengths and WeaknessesAs members of the General Surgery Editorial Board, a rigorous assessment of methodological strengths and weaknesses is essential to determine the clinical relevance and reliability of these findings.A. Methodological StrengthsThe primary strength of employing Mendelian Randomization lies in its capacity to address the limitations inherent in conventional observational studies. Minimization of Confounding Bias: The MR study design utilizes genetic variants (SNPs) as instrumental variables, exploiting the random allocation of these variables at conception. This genetic randomization effectively simulates a randomized controlled trial (RCT) by ensuring the exposure (genetic predisposition to constipation) is independent of typical lifestyle and environmental confounders (e.g., smoking, socioeconomic status, diet) that are typically correlated with both constipation and CRC risk. This design bypasses the systematic biases that inflate associations in standard epidemiological research. Rigorous Assessment of Reverse Causation: The bidirectional nature of the study provides crucial evidence that addresses a major clinical ambiguity. Many observational studies cannot distinguish if constipation is a risk factor or merely an early symptom of pre-existing, undiagnosed CRC. By explicitly testing the hypothesis of CRC \rightarrow Constipation, the MR analysis found no causal effect. This finding solidifies the understanding that constipation, if associated with CRC, acts as a potential precursor rather than a consequence. Instrumental Validity and Statistical Power: The selection of genetic instruments was robust, requiring a high F statistic (>10) for each SNP, thereby confirming the strong association between the instruments and the exposure phenotype (constipation). This methodology ensures that the estimation of the causal effect is not undermined by weak instrument bias. Triangulation of Analysis Techniques: The use of multiple complementary MR methods (e.g., IVW, MR-Egger, Weighted Median) allows for rigorous sensitivity analyses regarding pleiotropy—the phenomenon where a genetic variant affects the outcome through pathways other than the intended exposure. While the results were ultimately divergent, the attempt to triangulate findings enhances the overall scrutiny applied to the data.B. Critical Weaknesses and LimitationsDespite the sophistication of the MR approach, several limitations significantly challenge the conclusion that chronic constipation is a definite causal factor. Lack of Statistical Robustness Across Methods: This is the most critical weakness. Although the IVW-random effect analysis suggested a marginal causal link (OR 1.002), the failure of the other four sensitivity MR approaches to confirm this association raises concerns. The discrepancy strongly suggests the presence of horizontal pleiotropy, meaning that the genetic variants selected for constipation may also influence CRC risk via an unmeasured biological pathway (e.g., general inflammatory or metabolic processes) that is independent of changes in bowel habits. This possibility renders the weak causal claim highly tenuous. Clinically Trivial Effect Size: The reported Odds Ratio of 1.002, while achieving technical statistical significance (P = 0.023), possesses no meaningful clinical significance. Fora General Surgery Editorial Board focused on identifying targets for screening or intervention, a risk factor with such a marginal effect size is not prioritized, especially when compared to high-impact modifiable risk factors such as obesity or smoking. Absence of Subsite Specificity: The causal signal vanished when the investigators partitioned the outcome into colon cancer and rectal cancer. If the primary mechanism linking constipation to CRC were the prolonged contact time between potential carcinogens and the colonic mucosa (a widely hypothesized mechanism ), one would expect the effect to be spatially consistent, particularly in the distal colon where transit is typically slowest. The lack of an effect in anatomically defined subsites suggests that the weak overall "CRC" result is likely non-specific or due to residual statistical artifacts. Imprecise Phenotype Definition: MR studies rely heavily on the definition of the exposure phenotype in the source GWAS. Constipation in these large cohorts is typically defined broadly, often based on patient self-report or prescription records (e.g., \ge 2 laxative prescriptions). This broad definition fails to differentiate clinically relevant constipation subtypes, specifically slow-transit constipation—which is the type most mechanistically linked to increased carcinogen exposure—from functional constipation or outlet obstruction. The inclusion of diverse constipation phenotypes likely dilutes any true biological risk that might be confined to a specific, high-risk endophenotype.A comprehensive understanding requires contextualizing the MR findings against the spectrum of observational and controlled studies, highlighting the profound impact of confounding control.A. Compari
By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link: https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineData-driven surgery marks a crucial evolution in modern medicine, characterized by the use of measurable evidence and individualized patient metrics to guide surgical decision-making and optimize outcomes. This approach moves beyond generalized surgical protocols toward personalized risk management tailored to the patient’s specific anatomy, metabolic health, and long-term needs.Key aspects of data-driven surgery, supported by recent research, include leveraging simple patient characteristics, challenging surgical dogma, utilizing predictive models, and adopting new technologies for customization: 1. Simple Data Informing Surgical TechniqueIn routine procedures, simple, measurable data is used to stratify risk and select the safest approach: Subcutaneous Fat Thickness (SFT): Studies involving thousands of patients have established SFT (the thickness of the fat layer under the skin) as a powerful predictor of post-operative infection risk. For patients with increased SFT undergoing a traditional open appendectomy, the risk of Surgical Site Infection (SSI) was found to be 1.82 times higher (nearly double). Crucially, this data dictates a personalized approach: if the surgeon opts for the laparoscopic (keyhole) procedure, the SSI risk is not significantly higher even with increased SFT (risk increase of only 1.09x). This provides a clear, actionable game plan: Measure SFT pre-operatively, and if it is high, strongly consider the minimally invasive route to lower the patient’s individual risk of infection. 2. Utilizing Predictive Modeling and Metabolic MarkersData-driven surgery relies on sophisticated tools, including machine learning and metabolic markers, to predict individual patient risks: AI Risk Calculators: Tools like the Potter Predictive Optimal Trees in Emergency Surgery risk calculator use machine learning to provide transparent, accurate, and actionable risk assessments for emergency laparotomy patients. Validation studies demonstrated its high accuracy in predicting 30-day mortality (C statistic = 0.90) and complications like septic shock and respiratory failure. This early warning allows clinicians to initiate proactive, targeted management sooner (e.g., optimizing fluids or considering antibiotics), potentially avoiding severe complications or high-risk surgeries later on. Metabolic Markers: Metabolic health insights are integrated into pre-operative risk profiles, even in oncology. The Triglyceride Glucose (TAIG) index, which correlates highly with insulin resistance, is being investigated as a potential diagnostic aid. The TAIG index has shown a moderate ability (pooled area under the curve of 0.64) to help differentiate between malignant (cancerous) and benign (non-cancerous) breast lesions. Although not strong enough to be a standalone diagnostic tool, combining this metabolic data with imaging and biopsy findings helps create a more comprehensive and personalized risk profile for the individual patient before surgery. 3. Data Challenging Surgical DogmaData is essential for maintaining surgical integrity and ensuring the best long-term outcome for the patient, even if the evidence contradicts the prevailing dogma of choosing the least invasive option: The Thymus Gamble: In the case of aggressive chest tumors (thymic carcinoma), data showed that pre-operative scans were highly unreliable, with almost 80% of tumors appearing early stage actually being more advanced upon removal. Researchers found that patients who received the less invasive partial removal had significantly worse overall survival rates (dropping from 67% to 30%) compared to those who received the more extensive total thymectomy. In this high-stakes scenario, the evidence makes it clear that total thymectomy is "oncologically superior," demonstrating that the choice must be guided by definitive, hard, long-term evidence—even if it means opting for a bigger, more aggressive operation. 4. Data Reframing Major Surgery as PreventionLarge-scale, long-term data sets are used to evaluate the impact of surgery as a proactive, durable risk mitigation strategy: Bariatric Surgery: Data supports reframing bariatric surgery less as a last-resort treatment for obesity and more as a proactive defense against a lifetime of chronic illness, offering a systemic metabolic reset. A massive study showed that the surgery group had a nearly 80% lower risk of developing Type 2 Diabetes later on, and substantially reduced risks for hypertension (almost 59% lower), high cholesterol (50.5% lower), and obstructive sleep apnea (nearly 57% lower) compared to the control group. This data provides a durable approach for risk mitigation and supports considering surgery as a potential "best first move" for carefully selected patients. 5. Data Guiding Real-Time CustomizationThe ultimate form of data-driven surgery involves customizing solutions at the moment of the procedure using advanced technology: Portable 3D Bioprinting: Handheld 3D printers, often called a "bone glue gun," allow surgeons to extrude a custom scaffold directly into complex bone defects. The "bio-ink" material (a composite of polycaprolactone, PCL, and hydroxyapatite, HA) can be customized on the fly. The surgeon can adjust the ratio of PCL-to-HA to tune the final scaffold's properties, such as its mechanical strength and how quickly it degrades, directly addressing the unique load-bearing requirements and specific biological needs of that particular bone defect in that patient. By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineTo access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
منابع گردآوری شده یک بررسی انتقادی از عمل زنان و زایمان زیبایی به نام واژیلآنجلو (Vagilangelo) ارائه میدهند، که ادعاهای بازاریابی آن را در تضاد با نگرانیهای جدی اخلاقی و علمی قرار میدهد.بررسی انتقادی عمل واژیلآنجلو (Vagilangelo): ادعاها، نگرانیها و نیاز به اصلاحاتادعاهای بازاریابی و نوآوری معرفی شده:مواد تبلیغاتی و اسناد مرتبط با واژیلآنجلو این عمل را به عنوان یک "پیشرفت انقلابی" در حوزه جوانسازی واژن توصیف میکنند. این رویکرد پیشگامانه ادعا میکند که جنبههای ساختاری و عملکردی سلامت واژن را با ترکیب مکانیسمهای زیر بهبود میبخشد:1. بخیههای داخلی و تنظیم بیومکانیکی: این روش برای بازیابی زاویه طبیعی واژن که ممکن است به دلیل تأثیرات پیری یا زایمان تغییر یافته باشد، از بخیههای داخلی استفاده میکند.2. طب ترمیمی (PRP/اگزوزومها): این تنظیمات با استفاده از پلاسمای غنی از پلاکت (PRP) و اگزوزومها ترکیب میشود که ظاهراً برای تحریک بازسازی بافت و افزایش حساسیت یا رضایت جنسی عمل میکنند. این امر به عنوان راه حلی جامع برای احیای اعتماد به نفس و شادابی در زندگی جنسی بازاریابی میشود.انتقادات علمی و اخلاقی جدی:در مقابل ادعاهای تجاری، چندین منبع تحلیلی قویاً استدلال میکنند که واژیلآنجلو یک روند نگرانکننده از "استثمار" در حوزه رو به رشد جراحی زیبایی زنان جهانی را تجسم میبخشد. این انتقادات بر اساس فقدان کامل شواهد علمی و خطرات بالقوه ساختاری است: فقدان دادههای مبتنی بر شواهد: این عمل فاقد "دادههای داوری همتا شده" (peer-reviewed data) است که سازوکارهای آن یا نتایج ادعا شده آن را تأیید کند. ایمنی نامشخص طولانیمدت: هیچ کارآزمایی کنترلشده تصادفی یا دادههای ایمنی طولی معتبری فراتر از چند ماه (یا صفر فراتر از ۶ ماه) وجود ندارد. این امر اصول اساسی "پزشکی مبتنی بر شواهد" و رضایت آگاهانه را نقض میکند. خطرات بخیههای داخلی: مشخصات خطر واژیلآنجلو به طور خطرناکی تعریف نشده باقی میماند. خطرات نظری ناشی از بخیههای داخلی که در نزدیکی ساختارهای ظریف عصبی-عروقی قرار میگیرند، شامل احتمال آسیب به عصب، ایجاد مقاربت دردناک (دیسپارونی)، یا آسیب به مثانه یا مجرای ادرار است. عدم استانداردسازی PRP: استفاده از PRP در این کاربرد فاقد شواهد خاص بافتی برای کارایی است و پروتکلهای تزریق آن فاقد استانداردسازی هستند.اثر تشدیدکننده گردشگری پزشکی و آموزش غیراخلاقی:این بحث و جدل به دلیل وجود یک اکوسیستم استثماری که توسط پارادایمهای آموزشی غیراخلاقی و گردشگری پزشکی کنترل نشده تغذیه میشود، پیچیدهتر میشود: دورههای آموزشی کوتاه مدت و بدون اعتبار: برنامههای آموزشی برای این روش در حد ۳ تا ۵ روز، عمدتاً در کشورهای عربی، گواهی جراحی صادر میکنند. این مدت زمان به شدت با ۱ تا ۲ سال آموزش نظارتشده مورد نیاز برای فلوشیپهای جراحی در کشورهای با درآمد بالا مغایرت دارد. بهرهبرداری از بیماران آسیبپذیر: بیماران آسیبپذیر، اغلب زنان پس از زایمان یا افراد کمدرآمد در مناطقی مانند بحرین، ناخواسته تبدیل به "ماده تمرینی" برای پزشکانی با آموزش ناکافی میشوند. بار اقتصادی گردشگری پزشکی: گردشگری پزشکی، که در مقاصدی مانند ایران، مصر، و ترکیه رونق دارد، اغلب شامل بستههایی است که مراقبتهای پس از عمل معنادار را حذف میکنند و منجر به عوارضی مانند عفونت یا شکست ایمپلنت میشود. این عوارض سپس به سیستمهای بهداشت عمومی محلی تحمیل میشوند و بار مالی سنگینی ایجاد میکنند.درخواستها برای اصلاحات نظارتی و اخلاقی:منتقدان خواستار اقدام فوری برای جایگزینی سود با اخلاق هستند. توصیههای ارائه شده در منابع شامل موارد زیر است: تعلیق بازاریابی (موراتوریوم): درخواست برای تعلیق فوری بازاریابی واژیلآنجلو تا زمانی که کارآزماییهای تصادفی و کنترلشده (RCT) مناسب در برابر روشهای شم (Sham procedures) یا فیزیوتراپی لگنی منتشر شوند. اصلاح استانداردهای آموزش: ممنوعیت جهانی فلوشیپهای جراحی زیبایی که کوتاهتر از سه ماه هستند و اجرای حداقل دورههای اجباری که با الزامات فدراسیونهای جراحی (مانند FEBS) برای ادغام مهارتهای نظارتشده مطابقت داشته باشد (معمولاً ۲ تا ۳ ماه). نظارت و پاسخگویی: تقویت نهادهای اعتباربخشی ملی (مانند SAPSB و GMR عربستان سعودی) برای اعمال شفافیت در تبلیغات، مجازات برنامههای فاقد اعتبار، و اجباری کردن سیستمهای گزارشدهی عوارض جانبی. اولویتبندی اخلاق: به رسمیت شناختن اینکه تجاریسازی عدم قطعیت در سلامت زنان "استثمار" است و نه نوآوری، و لزوم اجرای سیاستهایی که اصول اخلاقی پزشکی (مانند primum non-nocere یا "اول آسیبی نرسان") را بر سود اقتصادی اولویت میدهند. Get full access to Reza Lankarani at lankarani.substack.com/subscribe
By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link: https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | @Genesis Journal of Surgery and Medicine------------------------------------------------------------International Journal of Surgery October 15, 2025 DOI: 10.1097/JS9.0000000000003600------------------------------------------------------------1. Overview: The study investigates whether partial thymectomy is oncologically acceptable for thymic carcinoma, a rare and aggressive subtype of thymic epithelial tumors (TETs). Using real-world multicenter data from 19 Japanese institutions (2010–2021), the authors analyzed 92 patients who underwent curative-intent resection—73 with total thymectomy and 19 with partial thymectomy. Key Methods: - Retrospective comparative cohort design. - Primary endpoints: overall survival (OS) and recurrence-free survival (RFS). - Statistical adjustment via overlap weighting to mitigate selection bias. - Central pathological review for diagnostic consistency. Key Findings: - 79.3% of clinical stage I cases were upstaged postoperatively, highlighting limitations of preoperative imaging. - In unadjusted analyses, partial thymectomy showed a trend toward worse OS and RFS (p ≈ 0.055–0.057). - After propensity-weighted adjustment, partial thymectomy was significantly associated with: - Worse OS (p = 0.0027) - Higher recurrence risk (p < 0.0001), especially early postoperative recurrence. - Local and distant recurrences were significantly more common in the partial group after weighting. Conclusion: Total thymectomy is oncologically superior for thymic carcinoma. Given the difficulty in preoperative differentiation from thymoma, total thymectomy should remain the standard for all resectable TETs unless a definitive benign diagnosis is confirmed.--- 2. Critical Assessment: Strengths and WeaknessesStrengths:- Multicenter real-world data: Enhances generalizability beyond single-institution bias.- Central pathological review: Ensures diagnostic uniformity—critical given histological complexity of TETs.- Advanced statistical methodology: Use of overlap weighting (superior to traditional propensity matching in preserving sample size and reducing variance) effectively balances baseline imbalances (e.g., age, stage, performance status).- Clinically relevant question: Addresses a growing dilemma as minimally invasive partial resections gain popularity for early thymoma.- Clear staging discrepancy demonstration: The Sankey diagram powerfully illustrates the high rate of understaging in clinical practice.Weaknesses:- Small sample size in partial group (n=19): Limits statistical power for subgroup analyses and increases vulnerability to outliers.- Retrospective design: Inherent selection bias—partial thymectomy patients were older, frailer, and had smaller tumors, suggesting surgeon preference for less aggressive surgery in higher-risk patients.- Lack of standardized partial resection definition: “Partial” included hemi-thymectomy and tumor-only resection, introducing heterogeneity.- No intraoperative frozen section use: While realistic (as noted in discussion), this reflects a missed opportunity to explore adaptive surgical strategies.- Limited external validation: All centers are in Japan; biological or practice-pattern differences may limit global applicability.--- 3. Comparison with Recent StudiesRecent literature largely supports partial thymectomy for early-stage thymoma but remains cautious for thymic carcinoma.Graphical Insight (Conceptual):Key Contribution: This is among the first robust multicenter studies to demonstrate that partial thymectomy is inadequate for thymic carcinoma, even when tumors appear early-stage. It cautions against extrapolating thymoma data to carcinoma.--- Academic Significance: This study makes a timely and clinically vital contribution. As minimally invasive surgery expands, there is a real risk of undertreating thymic carcinoma due to preoperative misclassification. The authors provide strong real-world evidence that total thymectomy is non-negotiable for optimal oncologic control in carcinoma.Impact: - Likely to influence guidelines (e.g., NCCN, ITMIG) to explicitly discourage partial resection when carcinoma cannot be ruled out.- Reinforces the need for caution in adopting partial thymectomy outside rigorously confirmed early thymoma.--- Plain-Language Summary for Patients and the Public If a tumor is found in the thymus (a small organ behind the breastbone), doctors often can’t tell before surgery whether it’s a slow-growing type (thymoma) or a more aggressive cancer (thymic carcinoma). Some surgeons have started doing smaller operations (partial thymectomy) for what looks like early, harmless tumors. But this study shows that if the tumor turns out to be thymic carcinoma, the smaller surgery leads to more recurrences and lower survival. Because it’s so hard to tell the difference before surgery, removing the entire thymus (total thymectomy) gives the best chance of curing the cancer, even if the tumor looks small and harmless on scans. ------------------------------------------------------------Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and MedicineTo access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link:https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe
Reviewed by Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link: https://surgicalpioneer.codeadx.me/ Get full access to Reza Lankarani at lankarani.substack.com/subscribe
By Dr Reza Lankarani, General SurgeonFounder | Surgical Pioneering Newsletter and Podcast Series Editorial Board Member | Genesis Journal of Surgery and Medicine To access additional details, please refer to the Surgical Pioneering Podcast Series application available at the following link: https://Surgicalpioneer.codeadx.me Get full access to Reza Lankarani at lankarani.substack.com/subscribe