Discover The PCOS Podcast
The PCOS Podcast

The PCOS Podcast
Author: Let's talk about our ovaries and the science of PCOS.
Subscribed: 0Played: 0Subscribe
Share
© The PCOS Newsletter
Description
Finding the truth about PCOS. Bringing you the true science of PCOS and women's health with expert guests and a ton of insights.
www.thepcosnewsletter.com
www.thepcosnewsletter.com
11 Episodes
Reverse
Hello everyone,Today I have the pleasure of introducing you to Dr Lily Kruse, a cardiac surgeon with a Yale medical degree and a deep passion for prevention. A deep conversation that will show you how to take care of your heart early so we can live a long, fulfilling life. We answer:* What are the differences between men and women in CVD?* Women are twice as likely to die of a heart attack compared to man. Why is that?* What symptoms should I take seriously as a women?* How does each hormonal stage in a women’s life impact our CVD risk?* How can I protect my cardiovascular health?* What is your view on PCOS in relation to CVD? This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone, Here we are! 2026 has officially started!You know I like to talk a lot about behaviour change in January, and this year I am bringing you an interview with Dr Rosie Webster, the person who first taught me about behaviour change in 2021.PS: The videos I upload here are available as podcasts on Spotify, Apple Podcasts or on YouTube. If you prefer reading, I have summarised the conversation below.If you have PCOS and feel stuck in cycles of motivation, burnout, and starting over, this episode is for you. We break down why common advice doesn’t work, why weight loss is such a frustrating goal, and how behavioural science can help you build habits that actually support your hormones, health, and long-term life. You’ll leave with a clearer way to think about habits, health, and January resets and a framework you can actually apply to your own life. We answer the following:* Why does motivation fade so quickly when we try to change our habits, especially around weight and lifestyle?* Why doesn’t “just trying harder” work when it comes to weight loss and behaviour change?* How should someone approach lifestyle change in a way that’s realistic and sustainable, rather than all-or-nothing?* What role do our environment and daily context play in why weight-related changes feel so hard to stick to?* Why does focusing on weight loss often backfire, and what should people focus on instead?* How can someone use a fresh start (like January) to actually set up changes that last long term?Rosie has a PhD in Health Psychology and is a behavioural science consultant and health coach, specialising in how people make and sustain health behaviour change. The perfect person to speak to in January, as we are considering making changes to our lifestyle for PCOS. If you’d like to get even deeper on the topic, Roise is doing a 7-day free email course called Resolutions Reframed. You can sign up here: www.reframehealth.uk/resolutions-reframed. Otherwise, she is also available on Instagram.Over to Rosie: Why is everyone starting fresh in January?There’s a reason January feels like such a decisive “reset” moment, and it isn’t just cultural, it’s psychological. Research on what’s called the fresh start effect shows that when we hit moments that feel like a new beginning (January, a birthday, even a Monday), we get a temporary spike in motivation. It feels like a clean slate. Past mistakes feel further away, and we feel more optimistic about who we can become.That motivation is real — but it’s also short-lived. The problem isn’t that people feel motivated in January. The problem is that we expect that motivation to carry us indefinitely, without changing anything else around it.Why do we run out of motivation?Most people approach lifestyle change by riding that initial motivation high. They decide they’re going to exercise more, eat differently, or completely overhaul their routine — often all at once. What’s usually missing is any real thought about how those changes fit into their actual life, or what happens when motivation drops, which it inevitably does.From a behavioural science perspective, behaviour isn’t driven by motivation alone. It’s driven by a combination of motivation, capability, and opportunity. If any one of those is missing, change becomes very hard to sustain. This is the COM-B model. What is the COM-B model and why is it the only way to change behaviour?Behaviour is driven by Capability, Opportunity, and Motivation.CapabilityCan I realistically do this?* Do I have the knowledge or skills?* Am I mentally overloaded or exhausted?* Do I know how to do this safely?Sometimes the blocker isn’t laziness — it’s overwhelm.OpportunityDoes my environment support this?* Is it physically easy to do?* Does my social environment help or hinder me?* Is it convenient, accessible, and realistic?If something requires constant friction, it’s unlikely to stick.MotivationDo I want to do this — not just feel like I should?* “I should do this” is weak motivation* “I want this because it matters to me” is far strongerWhen people struggle, it’s rarely because they “lack willpower”. It’s usually because one of these pieces hasn’t been properly thought through.AAn example Let’s say I want to strength train twice a week.Capability:If I don’t know how to lift weights safely, or I feel intimidated, that’s a real barrier.Opportunity:If the gym is 20 minutes away, no one I know goes, and it doesn’t fit my schedule — that’s another barrier.Motivation:If I’m doing it because my doctor said I should, that motivation will fade.If I’m doing it because I want to feel strong, independent, and confident as I age — that’s much more powerful.The key is balancing all three, not forcing one.Our environmentOne thing I think we massively underestimate is how much our environment shapes our behaviour. We live in a world that constantly nudges us towards convenience, food availability, and inactivity. Against that backdrop, we’re often told that our health outcomes are purely about personal responsibility.When behaviour change doesn’t stick, people tend to blame themselves. But the reality is that many of the forces acting on our behaviour are completely outside our control. Recognising that doesn’t mean giving up — it means being kinder to ourselves and more realistic about what change actually requires.Rather than asking, “Why can’t I stick to this?”, a more helpful question is, “Given the life and environment I actually have, what’s realistic for me right now?”Why chasing weight loss usually doesn’t end wellThis is where my perspective can sometimes feel uncomfortable, especially for people who’ve been told for years that weight loss is the solution to their health problems.In most cases, I don’t recommend pursuing weight loss as the primary goal. That’s not because weight never changes — it often does — but because focusing on weight tends to push people into restriction, extremes, and a constant battle with their own body.When people try to lose weight, they often have to eat less while feeling hungrier, exercise more while feeling more tired, and ignore signals from their body that something isn’t sustainable. Biologically, the body responds by increasing hunger hormones and slowing metabolism, because it’s trying to protect you. That’s why weight loss so often leads to weight regain. It’s not a lack of discipline — it’s physiology.Instead, I encourage people to focus on behaviours they actually have some control over: how they eat, how they move, how they care for their body day to day. Those changes improve health regardless of whether weight changes, and they’re far more likely to last.Why All-or-Nothing changes rarely workExtreme approaches — cutting out entire food groups, rigid rules, dramatic overhauls — can feel appealing because they’re clear. You know exactly what you’re allowed to do and what you’re not. But clarity doesn’t equal sustainability.What works better, almost every time, is making smaller changes and building on them gradually. Changes that feel good in your body. Changes that don’t require you to constantly fight yourself. Over time, those small shifts add up — not just physically, but in how you relate to your health.Why change feels so hard Our brains are designed to rely on habits because habits save energy. Changing behaviour requires conscious effort and self-regulation, and that’s tiring. When that effort runs out, we default back to what’s familiar — not because we’re lazy, but because it’s efficient.That’s why I often say that when people “fall off the wagon,” it’s because the wagon was never built to last in the first place. The solution isn’t more willpower. It’s better planning, better design, and more compassion.How to use January in a way that actually helpsJanuary motivation can be incredibly useful — but not if it’s spent trying to do everything at once. I’d much rather see people use that energy to slow down and do the groundwork properly.That means reflecting on what truly matters to you, what kind of life you want to support, and which behaviours help or hinder that. From there, you can start identifying small, meaningful changes that feel supportive rather than punishing.It also means making plans that can flex. Life is unpredictable. If one approach doesn’t work on a given day, the goal doesn’t disappear — you just find another way to meet it.A final thoughtLasting change doesn’t come from forcing yourself into a new identity overnight. It comes from understanding yourself better, designing for the life you actually live, and choosing changes that feel good enough to keep doing.That’s where real sustainability lives.Thank you so much to everyone for tuning in. See you in 2 weeks!Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone,Today, I bring you another PCOS story from Dr Laura. She was sent home at 18 years old with a diagnosis of menopause, instead of PCOS and no answers.Dr Laura hosts her own PCOS podcast, Triggered by Testosterone, where she speaks openly about PCOS, hormones, mental health, and the realities of managing this condition in everyday life. Laura holds a PhD in Management Studies, where her work focuses on women’s health in the workplace and how organisations can better support women living with chronic and hormonal conditions. Her academic research is profoundly shaped by her own experience navigating PCOS. This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone, Caroline’s 10 years learning regarding her fertility and PCOS were so touching. Listening to her has made me feel angry, hopeful and determined. Sharing these insights will help so many women avoid the pain of having to try for 3 years before conceiving. This episode is also dear to me because it showcases how tools such as ovulation trackers, knowledge and advocating for yourself can help women navigate this challenging time that some of us have to go through.Weather you are just starting your conceiving journey, have been in it for a while or want to know what tools to use once the times comes, this episode is for you.Ultrahuman gifted me their product for review; this interview is part of that collaboration. Caroline goes through her realisation that she had a short luteal phase using the OvuSense vaginal temperature tracker and how she had to fight for ovulation medication due to her weight. A story of resilience, perseverance and love. Caroline is part of the Ultrahuman team, who have recently acquired viO HealthTech company who produces the OvuSense temperature trackers. She left her job at a police department to join this team because of how much she believes in advocating for women with PCOS. The Ultrahuman team has a 30% discount on their ring who has an advanced temperature tracking module. I don’t gain any monetary value from sharing this. Have a good Sunday,Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone,This article was quite hard to write and film emotionally. For anyone who wishes to become a mother, the thought of managing to get pregnant and losing it is terrifying. I have added one more episode to the series. So far we have gone through:* Episode 1: PCOS and fertility - how do I know how much time I have left?* Episode 2: How can I prepare my body for pregnancy?* Episode 3: The other side of the coin -> checking your partner’s fertility and optimising for a family* Episode 4: Finding ovulation when your cycles are irregular* Episode 5: The risk of miscarriage I know numerous women who have gone through miscarriages and then went on to have healthy babies later down the line, or women who needed assistance. The reason why I think it’s important to talk about it is because it normalises it. 90% of miscarriages in the first trimester are down to chromosomal problems - so it’s not your fault if it happens. Many women blame themselves for it, but it’s a natural phenomenon. Of course, we are emotionally intelligent animals, so it’s hard to stay purely in the facts, but understanding the odds is helpful. Approximately 25% of women experience a miscarriage in their lifetime, so that’s 1 in 4 who will have to go through this unpleasant experience. I have been very close to two of my friends’ miscarriages and their experience, which, while painful, normalised it. Here are the numbers for women without PCOS and those with PCOS.❤️ This content is for our paid subscribers. A lot of work and research goes into writing these articles. Consider becoming a paid subscriber to get the most scientifically-backed PCOS information and learn to control your PCOS. Women without PCOSThere is a book that provides in-depth details about the data we have on popular pregnancy myths. It’s called Expecting Better by Emily Oster. I can see that she was a very anxious mom-to-be and found a lot of comfort in understanding risk percentages and delving deeply into the data. If you are seen at week 6, and everything looks good, these are the % of pregnancies that are lost afterwards. Starting at 11% in week 6 and going down to 2% in week 11. A very sharp decrease.Other sources, such as the Tommys, a charity dedicated to pregnancy and babies, report the following numbers: early miscarriages happen to 10-20 in 100 (10 to 20%) of pregnancies. That’s almost 1 in 5. Second-trimester miscarriages happen in 3-4% of pregnancies. The numbers differ according to the source. As you can imagine, it’s pretty hard to estimate, as some of the miscarriages can go unnoticed when they happen. Some studies even put the risk at week 3 at 30%. The risk of losing your pregnancy goes down as time passes and the little cells become a fetus. Women with PCOSIt will come as no shock to you that we have a higher chance of miscarriage. With this condition, you can pretty much assume that we have an increased risk of every disease under the sun. It does show the wide range of implications of hormones on our bodies. A paper on pregnancy in women with PCOS puts our first-trimester miscarriage rate between 30 to 50%. It is pretty challenging to determine, so most of these figures come from studies where some form of assistance was provided. For example, treatment with ovulation-inducing agents such as clomiphene or letrozole is associated with a higher incidence of miscarriage compared to the naturally conceiving population. It is not known the rate of miscarriage for those who conceived naturally. I guess that it depends heavily on how well-controlled your PCOS is. Why?1. Increased LHAn increase in LH characterises PCOS. High LH can:* Prematurely trigger oocyte maturation → poorer quality eggs.* Impair corpus luteum function → insufficient progesterone support for early pregnancy - progesterone is needed for the endometrium to develop and be stable where the embryo implantsWhat can I do?Before conceiving, it would be ideal to undergo a test to determine your baseline LH levels. Elevated LH is primarily genetic; however, there is evidence that insulin can increase LH secretion - so taking care of your insulin levels MIGHT*** help.Might*** - with three *** because it’s very hard to prevent miscarriages or be sure of what the issues are - the things that I suggest are in no way saying - if you do this, you won’t have a miscarriage. As we saw at the beginning of this article, most of it’s chromosomal - we are just trying to understand if the percentage increase compared to women without PCOS might be due to PCOS-specific things. I am a control freak - so if there are things that I can try, I will do them even though they might not necessarily have an effect. 2. Elevated androgensElevated free/total testosterone ratios were found to be predictive of early pregnancy loss in two different studies.The authors speculated that high androgen levels antagonise estrogen, which may affect endometrial development and implantation. The endometrium is incredibly important for the embryo to implant and find its cosy home for the next 9 months. What can I do?Similarly, testing your testosterone levels beforehand is probably a good idea. It’s all about understanding your baseline and giving yourself 3-12 months prep time. We discuss how to prepare for pregnancy at length in our second episode. 4. Plasminogen activator inhibitor-1 (PAI-1) High plasminogen activator inhibitor-1(PAI-1) activity is associated with recurrent pregnancy loss in women with unexplained recurrent miscarriages. It has also been found to be significantly higher in women with PCOS. PAI-1 inhibits fibrinolysis - the body’s ability to dissolve clots. Tiny clots can form in the blood vessels that feed the placenta (the organ that supplies the baby with oxygen and nutrients). These clots block the blood flow, so the placenta doesn’t get enough circulation. Without proper blood supply, the placenta can’t support the baby → leading to pregnancy loss.What can I do?There is a study which documented improved pregnancy outcomes with metformin in overweight women with PCOS and correlated it to significantly reduced PAI-1 activity levels resulting from treatment. This is an option. Metformin will come up later in the article. 5. Insulin Resistance You knew this one was coming. This one has multiple implications:* Alters oocyte quality and maturation.* Interferes with glucose uptake in the endometrium → poor energy support for implantation.* Exposure to excess glucose can turn on a “self-destruct switch” ( apoptosis) * Suppresses GLUT4 expression in endometrial cells, reducing glucose transport.* Reduces glycodelin & IGFBP-1 (proteins crucial for implantation and maternal immune tolerance).What can I do?Allowing yourself time to adjust your diet before trying to conceive is important. Metformin can also be your friend in these instances, together with Inositol, a low-GI diet and muscle building. 6. Endometrial DysfunctionEven beyond hormones and insulin resistance, women with PCOS may show:* Reduced β3 integrins → cell adhesion molecules needed for embryo attachment.* Reduced glycodelin → supports placental development and immune modulation* Reduced IGFBP-1 - regulates fetal growth and implantationCan I do anything to prevent a miscarriage?There is a retrospective review where 65 women with PCOS who continued metformin during pregnancy had a much lower rate of first-trimester loss (8.8%) compared to 31 women who did not take it (41.9%). Among those with a history of miscarriage, the protective effect was even more substantial (11.1% vs. 58.3%). These findings suggest that metformin use in pregnancy may significantly reduce early pregnancy loss in women with PCOS. There is a current research study ongoing, called the LOCIS Trial, which is due to be published later this year. The LOCI trial will generate robust evidence on whether continuing metformin treatment throughout the 1st trimester can reduce the risk of miscarriage for approximately 1,800 women with PCOS.I would discuss this with your doctor and consider taking Metformin for a while before you start conceiving and throughout your first trimester. Lifestyle and weight management are universally recommended and provide broader health and fertility benefits. Looking after our PCOS markers is essential. Supplementation with Vitamin D, Omega-3, and Folate is also very important. A good prenatal multivitamin can help. If you need specialised support, don’t hesitate to contact me at francesca.abalasei@gmail.comThis concludes our fertility series. I will create a lot more pregnancy content later on. I hope this has offered you a window into what you need to know about this chapter in our lives.See you next Sunday,Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone,I am so excited for this episode! I have tracked my ovulation for the past six months using four different methods to determine my ovulation window. In this video/article, I review the methods and analyse my 6 months of data, including an irregular 44-day cycle. This is useful for those trying to conceive, trying to avoid pregnancy, or trying to understand if they ovulate during their irregular cycles. As a reminder, this is a five-part series to deep dive into our ability to conceive.* Episode 1: PCOS and fertility - how do I know how much time I have left?* Episode 2: How can I prepare my body for pregnancy?* Episode 3: The other side of the coin -> checking your partner’s fertility and optimising for a family* Episode 4: Finding ovulation when your cycles are irregular* Episode 5: The risk of miscarriagePS: the articles are both in video and written format to fit both preferences of consuming information.Exclusive for members: This in-depth article is part of our premium content. Subscribers enjoy comprehensive PCOS deep-dives, customised meal plans, expert medical insights, and direct access to ask me questions.You can either subscribe monthly or purchase access to this article only.The four ways I used to find my ovulation* Skin temperature with Oura* Temperature with Natural Cycles* Vaginal temperature with OvuSence * Leutenizing hormone with LH stripsSkin TemperatureFor this, I used the Oura ring. This is the most straightforward method for tracking your ovulation. You only need to wear the ring and charge it. You can easily see when your temperature shifts upwards. This is due to progesterone. As soon as we ovulate, progesterone takes over to thicken the endometrium, and with this, a temperature increase occurs.The only downside is that skin temperature is considered less accurate than basal or vaginal temperature; however, after using it for a few months and establishing a consistent pattern, you can rely on it with greater accuracy. However, it is not studied for accuracy. Natural Cycle AlgorithmFor this, I have connected the Oura ring to this. Natural Cycles has an FDA-approved algorithm for contraception. They also send you the manual thermometer. Overall, the Natural Cycles detected ovulation one day after Oura, so they were pretty close. In the Natural Cycles app, you can also track your mucus, which is another way to know if you are ovulating and use LH strips. Unless you use the normal thermometer, I found this a bit useless overall. LH StripsLH strips work on Luteinizing hormone, which is the problematic hormone for us. Luteinizing hormone triggers ovulation when it is released, so it is at its highest 24-48 hours before ovulation. By peeing on one of these strips, you can detect when LH peaks:Women with PCOS are known to have higher LH levels - this means our LH peaks multiple times throughout the month without reaching the threshold needed for ovulation. Like this:However, if you have regular menstrual periods, this is an excellent way to confirm ovulation. Here is a surge I had in January.The challenge with this method is that it depends on when you take the test, the concentration of your urine and trying to catch this surge. Sometimes it doesn’t detect it like this cycle here: Vaginal TemperatureLastly, I tried Ovusense [not sponsored]. This weird device that you insert into your vagina at night takes readings throughout the night. I only managed to wear this for one cycle.I am personally not one who uses tampons, so for me, this was extremely uncomfortable to wear. They advertise specifically for PCOS, as vaginal temperature may be a bit more accurate at identifying temperature changes. They don’t have studies on their device done specifically on women with PCOS, so I'm not sure how true that is. For the cycle that I used it on, it detected my ovulation well. My dataThe methods identified by ovulation are slightly different days, but always on the 16/17/18th day mark. I don’t expect these to be 100% accurate, and I found that knowing this is more or less when I ovulate is super helpful.I did have a very irregular cycle of 44 days when I only ovulated on day 30. Just because you have 40-day cycles, it doesn't mean you can’t conceive if you manage to catch the ovulation window, so it may be useful to know when you are ovulating, as you can get pregnant even with irregular cycles. It’s also helpful to know so you can tell when your period will come, as the luteal phase is usually 10-15 days long.My recommendationsIf you can afford it, the Oura ring is the easiest and most comfortable to use; however, it might not be the most accurate. If you have irregular cycles and you are trying to conceive for a prolonged time, I would recommend the Ovusense paired with LH strips. You can also take your temperature normally with a thermometer in your mouth every morning before getting out of bed. This is the oldest and cheapest method. I find the effort involved in that a bit much, but if you can gain the habit of doing it every morning, it’s also an accurate measurement.I hope you enjoyed this article.See you next Sunday, Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone, I am bringing you a bit of an interesting article this week. Can men have PCOS? Well they don’t have ovaries so by default they can’t have PCOS. However in recent research PCOS-like symptoms has been noticed in male. Recent large-scale genetic research using data from the UK Biobank has provided strong support for the idea that men can develop a condition with features similar to PCOS, even though they don’t have ovaries. In a major study involving over 176,000 men, researchers found that those with genetic changes similar to those seen in PCOS were more likely to have obesity, type 2 diabetes, coronary artery disease, and early-onset hair loss. These findings held true in another large group of men from the Estonian Biobank, confirming that the pattern is real and not just a coincidence.If you're ready to invest in your well-being, consider becoming a paid subscriber. Your subscription gives you exclusive access to deeper insights, expert guidance, and the tools you need to feel your best. Let’s take this journey together!The main symptom: Early-onset androgenetic alopecia before the age of 35, aka early boldness. It looks like receding hairline and thinning at the crown, often forming an "M" shape.They also display low levels of sex hormone-binding globulin, increased free androgens, and sometimes paradoxically lower total testosterone compared to the normal range. If you want to catch up on what SHBG, for which we are also low in you can find the article below:In addition multiple studies show that men with early-onset AGA have a higher average body mass index (BMI) and are more likely to be overweight or obese than those without this type of hair loss. Higher BMI is significantly associated with greater severity of hair loss in early-onset AGA and in one study, men with early-onset AGA had a four times higher frequency of metabolic syndrome (which often includes obesity) compared to controls.Here we are, we are not the only ones having to go through hormonal rollercoasters. Unfortunately, brothers of women with PCOS and sons of women with PCOS often fall into this category, showcasing the PCOS is indeed a genetic condition. See you next Sunday,Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe
Hello everyone,Today, we have another episode of our fertility series. We bring in a very key component in conception: your partner. If you’re on a fertility journey with PCOS, chances are most of the focus has been on you - your hormones, your ovulation, your diet, your supplements. And yes, a lot is going on when it comes to managing PCOS. But fertility is a 50/50 partnership, and sometimes we forget to ask the important question: How’s the partner doing?In this episode, we answer important questions:* How does sperm production work?* Do men have a biological clock?* What tests should we do to assess men’s fertility?* What is important when it comes to sperm for optimal fertility?* What are the top things that affect sperm quality?* What are the top things men should pay attention to to give their sperm the best shot?* Is there anything special that male sperm needs to do for PCOS?As a reminder, this is a five-part series to deep dive into our ability to conceive with my colleague Daria, a Nutritional Therapist who specialises in fertility.* Episode 1: PCOS and fertility - how do I know how much time I have left?* Episode 2: How can I prepare my body for pregnancy?* Episode 3: The other side of the coin -> checking your partner’s fertility and optimising for a family* Episode 4: Finding ovulation when your cycles are irregular* Episode 5: The risk of miscarriagePS: the articles are both in video and written format to fit both preferences of consuming information.Exclusive for members: This in-depth article is part of our premium content. Subscribers enjoy comprehensive PCOS deep-dives, customised meal plans, expert medical insights, and direct access to ask me questions. Invest just £1.74/week in understanding and managing your PCOS effectively.How does sperm production work?Male sperm takes about 75 days to mature. The process starts in the seminiferous tubules in the testicles under the influence of FSH (follicle-stimulating hormone) where the sperm is produced. Production involves various stages (spermatogonial, spermatocyte and spermatid) and takes around 64 days. At the end of it, sperm cells have a tail and hopefully the correct number of chromosomes. After 64 days, those sperm cells travel into the epididymis, which is a highly-coiled tube attached to the testicles, where they spend a further 10-14 days gaining motility and the ability to fertilise an egg.Do men have a biological clock, too?Yes absolutely age does affect male fertility. Although the effects are not as pronounced as for women and there is anecdotal evidence for men who father children in their 90’s that is actually really quite rare. A large 2015 study analysed over 10,000 samples using DNA and found the oldest father to be 65,4 years old. There is however a woman who conceived naturally and gave birth to a son at the age of 59 if we were to look for outliers.When we look at more of an average population picture some research suggests that male fertility starts to decline from 30. The reality is that the older the man, the higher the chances for them to have suboptimal semen parameters, higher levels of DNA damage, poorer fertility outcomes and offspring health. A 2022 systematic review looking at fertility in ageing males, whilst recognising somewhat conflicting results of paternal age impact on fertility, found age negatively affecting nearly all semen analysis parameters, DNA fragmentation, risk of miscarriage and offspring genetic disorders in a lot of analysed studies. Another research looked at the time it took women to get pregnant and found that in couples where male partners were over 45 it took them 5 times longer to conceive when compared with younger males.Part of the reason the sperm quality is not given as much attention as it perhaps should is that a lot of male infertility factors could be overcome with ART (Assisted Reproductive Technologies) such as IVF (In-Vitro Fertilisation) and ICSI (Intracytoplasmic Sperm Injection). ICSI is a fertilisation technique used in IVF where a single sperm is injected directly into an egg.How do we diagnose an issue with man fertility?The good news about checking man fertility is that it is much easier to check the end product - the sperm itself which is regularly produced and easily connected, whilst it is almost impossible to assess the quality of the female egg directly. The main two tests to check male fertility are:* Semen analysis - this involves a sample of your partner’s semen being tested to check the amount of sperm in it. The test also checks how well the sperm moves, a parameter called motility and the shape of the sperm which is called morphology.* Semen DNA fragmentation - The human sperm cell, in fact, is not just responsible for the expression of the father’s genes but also for activation and the development of the embryo during and after implantation. This test checks for the occurrence of breaks in the long DNA chain, a.k.a. the presence of separated fragments of DNA.The above two tests are a good place to start. Conventionally the semen analysis would be done after 1 year of unprotected intercourse, and after 6 months when partners are 36 or over. If sperm parameters are abnormal other tests would be done to try and understand the root cause. This could include looking at man’s overall state of health including hormone levels such as LH and testosterone, blood sugar regulation and nutrients status amongst others.If there are established fertility issues it would be worth checking for infections and looking into seminal microbiome. Some infections such as Ureaplasma and Mycoplasma are often not causing any symptoms in men whilst potentially significantly reducing fertility. Some infections would decrease semen parameters whilst others might negatively affect female microbiome, decrease implantation chances and increase risks of miscarriage.What is important when it comes to sperm for optimal fertility?All the parameters that are measured in the semen analysis which is mentioned above are important. First let’s discuss what semen is because not all of the ejaculate or semen (what is expelled by the male partner during orgasm) is sperm cells. Semen is 60% alkaline seminal fluid containing nutrients, 30% thin milky fluid which again contains nutrients for energy production and also some molecules to increase sperm fluidity and only 10% sperm.Semen is analysed as a whole and various parameters are measured. Sperm count and concentration measures the number of sperm cells in a sample. It is of course important to have enough sperm cells in the ejaculate. Motility describes sperm ability to move or swim normally and progressive motility refers to the ability to swim in a straight line. It is one of the most important factors in male fertility as sperm cells need to have an ability to swim upstream in the female reproductive tract and also penetrate the egg. Morphology describes the size and shape of sperm when evaluated under the microscope. Most sperm cells are abnormal morphologically with current cut-off set at 4% meaning if a sample has 4% and over of sperm cells which have normal shape (and 96% are abnormal) the sample is regarded “normal” for this parameter. Other parameters would be tested as well such as semen volume and pH amongst others.Another really important parameter is how intact the DNA is inside the cell. In general if any of the semen parameters are suboptimal it correlated with higher DNA fragmentation. However, sometimes a man can have totally “normal” semen analysis as judged by the current criteria but an elevated DNA fragmentation score which is strongly correlated with poor fertility outcomes.What are the top things that affect sperm quality?(top 3) - maybe we can mention temperature, tight underwear (it seems a thing on the internet, not sure it’s a thing scientifically)There are so many! Age as we mentioned before, temperature of sperm production, dietary habits including consumption of refined carbohydrates and fat quantity and quality, lifestyle habits such as drinking alcohol and smoking, toxicity, medications, infections, general state of health and so much more. Which factors play the biggest role for each individual will vary based on their medical history, diet and lifestyle. Let’s start with the the temperatureSperm production works best at a temperature lower than the core temperature. Specifically, the optimal range for spermatogenesis is 34°C to 35°C, which is approximately 2–4°C lower than the normal human body temperature of 37°C. That’s why testes, which is the main site of spermatogenesis, are located outside of the body. This cooler environment is crucial for the development of healthy and motile sperm, as higher temperatures can impair sperm count, motility, and DNA integrity. One study compared semen parameters in healthy men who agreed to subject themselves to scrotal heating for 30-40 mins 2 days per week for 3 months. Sperm parameters such as sperm count, motility and morphology were decreased and DNA damage increased as a result of overheating.Certain medical conditions lead to overheating and are known to reduce fertility in men including undescended testes (when testes stay inside the body) or varicocele (varicose veins on testes which lead to increased blood flow and elevated temperature). A number of lifestyle factors contribute toward testicular heat including being sedentary for a long time, using a laptop on the lap, regular use of hot bath and sauna and tight clothing amongst others. Overexercising and cycling in particular could reduce semen quality and negatively affect fertility.Let’s talk about underwear. Tight underwear which brings testes closer to the body can indeed affect sperm quality. A 2012 study looked at the impact of wearing extremely tight underwear for 120 consecutive days in healthy fertile volunteers. They found that motility and viability of spermatozoa decreased whilst DNA damage increased as early
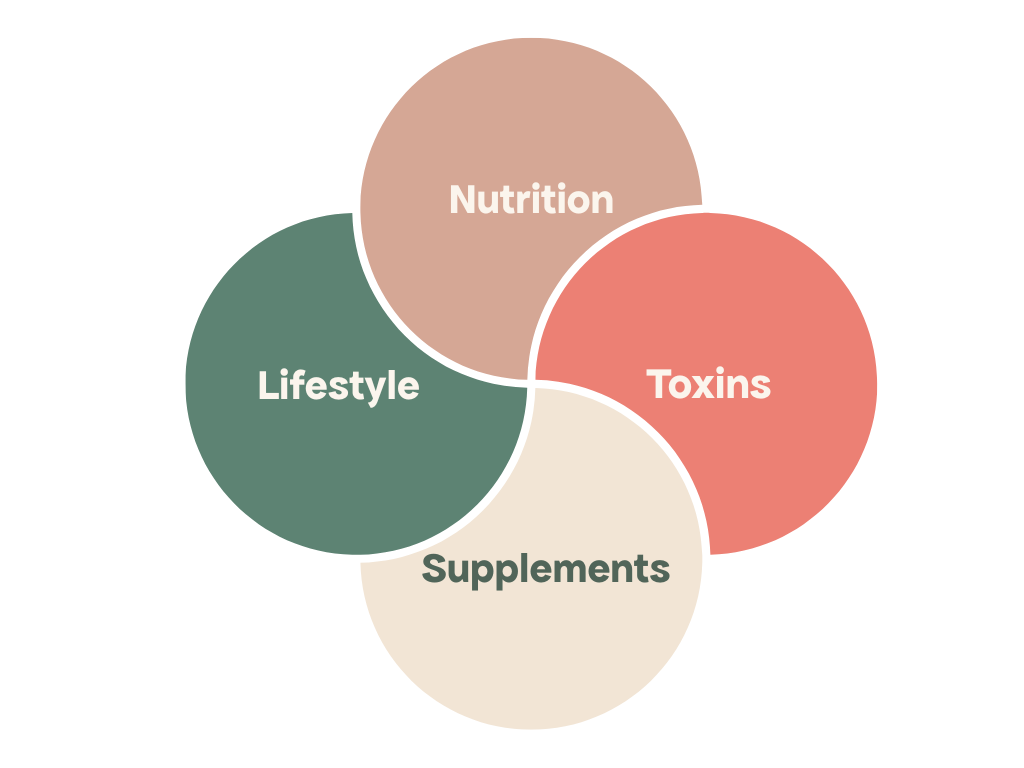
Hello everyone,Today I am bringing you Episode 2 of our Feritily series. As a reminder this is a five part series to deep dive into our ability to conceive with my colleague Daria, a Nutritional Therapist who specialises in fertility. * Episode 1: PCOS and fertility - how do I know how much time I have left?* Episode 2: How can I prepare my body for pregnancy?* Episode 3: The other side of the coin -> checking your partner’s fertility and optimising for a family* Episode 4: Finding ovulation when your cycles are irregular* Episode 5: The risk of miscarriage PS: the articles are both in video and written format to fit both preferences of consuming information.We discuss how to prepare your body for pregnancy using Daria’s four pillars:Exclusive for members: This in-depth article is part of our premium content. Subscribers enjoy comprehensive PCOS deep-dives, customised meal plans, expert medical insights, and direct access to ask me questions. Invest just £1.74/week in understanding and managing your PCOS effectively.Where should I start?When preparing for pregnancy with PCOS, adopting a mindset focused on long-term health for yourself and your future baby can make a significant difference. Instead of approaching this as a short-term effort, think of it as creating a foundation of health that benefits you and your family for years to come. This journey isn’t just about conception but about nurturing your body to thrive. PCOS can present unique challenges, but with the right approach, you can create a supportive environment for conception. In this article, we will discuss a realistic timeline for preparation and focus on four key pillars: nutrition, lifestyle, toxicity management, and supplements.Start thinking of yourself as pre-pregnantYour preparation for pregnancy begins well before conception. The cell that becomes your egg and later your baby undergoes critical changes in the few months before ovulation. Through a process called epigenetic changes, which is a change in gene expression a.k.a. genes being turned on and off, the state of health of future parents before conception has long-term effects on baby’s health even in adult life. This means that how you care for your body now directly influences your baby’s future health. Start treating yourself as you would during pregnancy: prioritising nutrition, rest, and overall well-being.How long before should I start preparing?The earlier you start, the better. The full process of folliculogenesis, where a primordial follicle develops into a preovulatory follicle ready for ovulation, typically takes about 10-12 months. The process starts to accelerate approximately 90 days before ovulation when the follicle evolves from secondary to pre-antral and starts growing more rapidly. In those 90 days, critical processing of the DNA occurs as well as differentiation in cells within the follicle. This is the window of opportunity to affect egg quality with nutrients, low levels of inflammation, and appropriate hormone levels. If you have less time, don’t worry as any amount of preparation is beneficial.The four pillars of fertilityTo optimise your chances of conception and ensure a healthy pregnancy, it’s essential to focus on the four pillars of fertility: nutrition, lifestyle, toxin management, and supplements.1. NutritionA nutritious, balanced diet is foundational for fertility, especially for women with PCOS. There is a lot of research about diet and fertility, diet and PCOS and less research about diet and fertility in PCOS.The Mediterranean diet has been shown over and over again to be beneficial for fertility in the general population. It lowers the risk of experiencing difficulty getting pregnant, improves chances of clinical pregnancy and live birth and improves sperm quality amongst others. The Mediterranean diet has also been shown to be beneficial for PCOS especially when combined with a lower carbohydrate consumption. A 2022 study looked at comparing a low-carbohydrate Mediterranean diet with a low-fat diet. Researchers looked at parameters such as body weight, fasting insulin and blood sugar, insulin resistance, blood lipids and various hormones including luteinizing hormone (LH), follicle-stimulating hormone (FSH), and prolactin (PRL) amongst others. After 12 weeks the Mediterranean diet group had more significant improvements in the menstrual cycle, normalising hormones, weight reduction and improving metabolic parameters.What about for fertility specifically?A 2021 systematic review looked at dietary interventions specifically aimed at fertility outcomes such as clinical pregnancy rates, ovulation and menstrual regularity and hormonal markers. 20 studies were included in the analysis. Interestingly, out of those 9 were investigating low-carbohydrate diet, 6 looked at low glycemic index/load diet, four evaluated DASH (Dietary Approaches to Stop Hypertension) diet and 1 trial looked at the Mediterranean diet. Overall these diets were shown to increase rates of clinical pregnancy, ovulation and menstrual regularity, reduce miscarriage rate and improve hormonal parameters. The degree to which diet affected which parameter varied amongst diets. For example both Mediterranean and low-carbohydrate were more-beneficial to pregnancy with improved clinical pregnancy rates and they also had more improvement on menstrual regularity. Por both of those parameters there was a strong correlation between treatment durations with effects becoming much more significant when participant followed the dietary pattern for over 3 months for pregnancy rates and 12 months for menstrual regularity.2. LifestyleYour lifestyle choices significantly impact fertility. Lifestyle includes things like the amount and quality of sleep that we’re getting, the exercise we’re doing, alcohol and caffeine consumption amongst others. One important thing to consider is your stress levels. It’s worth remembering that although sources of stress could be psychological, and they often are in modern life, they also could be physiological such as undereating, over exercising, inflammation, insulin resistance, imbalanced blood sugar, imbalanced gut microbiome and many others.Let’s see how stress can negatively affect fertility. When your body is stressed it shifts into the fight or flight response meaning the sympathetic nervous system is activated. Your body literally gets prepared to run away from the tiger or to fight it. Certain body functions get prioritised whilst others get slowed down. What gets prioritised is what is needed for your immediate survival - heart rate and blood pressure increase, more oxygen is coming through your lungs, glucose spikes in your bloodstream ready to be used by your muscles. What gets de-prioritised is your digestion, immune system and of course reproductive function.All these actions are achieved through hormonal activity. It’s primarily adrenaline, noradrenaline and cortisol from adrenal glands. Cortisol is a master hormone in the body meaning it can override the action of other hormones in the name of your survival. Let’s see how it affects reproductive function.* Excessive cortisol can interfere with the pulsatile release of gonadotropin-releasing hormone (GnRH), the hormone released by your brain which controls the menstrual cycle and ovulation, potentially leading to irregular or absent ovulation.* High cortisol levels can also inhibit the release of luteinizing hormone (LH) and follicle-stimulating hormone (FSH), affecting ovarian function and reducing the likelihood of pregnancy* Increased cortisol can lower preovulatory LH peak and estradiol levels, as well as post-ovulatory progesterone and estrogen levels, which can alter endometrial development and reduce the chances of conception* Cortisol dysregulation in PCOS can further exacerbate hyperandrogenism through impact on adrenal DHEA production as well as amplifying insulin resistance, which further stimulates ovarian androgen productionThe good news is that there is a lot that we can do to manage our stress levels and whilst some things are outside of our control a lot of things we have control over. Reducing stress is often closely linked with nervous system regulation which primarily involves lifestyle practices. Whatever you resonate with, be it breathing technique, time in nature, yoga, meditation, somatic movement, prayer, just incorporate it as a regular daily practice. Breathing is quite a good one to start because it is so closely linked to the rest-and-digest and fight-or-flight states of our nervous system. Even a few long and deep mindful breaths immediately after you wake up can make a huge difference to your stress levels in the morning. Better yet if you could do at least 10 minutes of breathwork per day.3. ToxinsToxins lead to disruption of endocrine (hormonal) health, increased level of inflammation, decreased cell energy production, damage to egg and sperm cells. We’re constantly exposed to various toxins, such as plastics, chemicals in our food and skincare, pesticides, heavy metals, and air pollution. The important thing with toxins is not to get overwhelmed and concentrate on some small manageable baby steps which you can do today to reduce your exposure.PhthalatesToday we’re going to concentrate on phthalates, which are chemicals found in many household products, cosmetics, and plastics. They are known as plasticizers meaning they increase the shape, flexibility, and durability of plastics, provide structure for products such as hairsprays and nail polish and help scents last longer in the fragranced products. Part of the problem with phthalates is that they are highly soluble in fats and not tightly bound to plastics, they can leach into food products - especially those high in fat, like milk, cheese, and oils.These chemicals are endocrine disruptors, meaning they can interfere with hormonal balance and potentially worsen symptoms of PCOS. Even in general population phthalates were s
Hello everyone, Death it’s a topic that no one wants to talk about. Very morbid, very uncomfortable, very sad. However, it’s the inevitable for all us humans. Let’s talk about it. If your first instinct reading the first paragraph was to stop reading, pause, and feel the uncomfortable. Happiness, progress and peace sits beyond our ability to face these feelings, not run away from them. In this article we will discuss the risk of 31 disease and answer the big question:Does having PCOS affect how long we can live?I debated weather I should make this a paid post. A lot of work and thought went into writing it and ensuring I present you with the right facts. However I think it’s such key information for all of you that I decided to keep it free. If you take value from my writing, I would appreciate if you’d upgrade to paid so I can continue bringing you high quality information about PCOS. I am part of a book club and January’s book was With the End of Mind by Kathryn Mannix, a palliative care doctor. The book goes through stories of people dying and the aim with her writing is to make people feel more comfortable with the thought of dying. The premise is that we made death clinical and dramatised through TV and soap operas. The process of dying was once something that we all withnessed but with the advancement of medicine we go through life not having seen someone dying. However she goes on to describe dying as she has experiences countless time in her career as peaceful, non-violent and natural. Unfortunately, I have already read my fair share of death books when my dad passed away. It was my first encounter with unexpected death. I had lost my grandmother before that but it was somehow expected. My dad was 50’s when he lost his life. At that time I found peace in reading stories of people who have gone through cancer diagnosis, spirituality and living through having a terminal diagnosis. At that time, I found them comforting as if I was sharing the pain with someone. This time around, reading this book was hard. It was challenging because I was now thinking of my own mortality and not my dad’s. If you chose to read it prepare for crying. Not a book you can read on public transport. A book that is uncomfortable but somehow needed to dismantle the taboo of death. This introspection made me think about our condition and how it impacts our longevity. We hear about all of the different diseases we have a risk for, but does having PCOS affect how long we can leave?I will tell you know that this research was hard to conduct. It’s very uncomfortable to think about your own trajectory. However it does help to understand why we must take care of our health and why our efforts in staying healthy are important. Let’s do some deep dive into the research.I looked into 5 different studies and there are some good news, some bad news and some conflicting news. The bad newsIf you are a half glass full person, maybe start with the good news.The bad news is that we have an increased risk of every disease under the sun (yay to us). This is a table from a study done from 2002-2018 in Alberta, Canada. It includes data from 16,531 PCOS cases and 49,335 age-matched non-PCOS cases (you might want to open this one on a computer). It is important to note that a 50% increase in risk is considerable but the prevalence if super important. For example, for Myocardial infraction (heart attack) our risk is 40% higher but it happens in about 0.55% of PCOS cases. Compared to infertility for which we have 4.5 fold higher risk and it happens in 27.03% of cases.I highlighted in yellow the ones that I think we need to pay attention to throughout our early life so we don’t suffer in our later life. As a result of the above there are some big areas we must work hard to lower the risk:* Infertility - we will explore this topic in depth this year through numerous articles * Excess testosterone - this affects all others including obesity, high cholesterol, endometrial cancer * Depression and Anxiety - extremely important to look after our mental health considering also the risk of more serious mental illnesses * Obesity - we know this by now and I don’t think I need to repeat it* Type 2 diabetes - this is one that goes hand in hand with obesity and insulin resistance.* High Cholesterol - testing and keeping an eye on this marker is extremely important for us * Endometrial Cancer - I will write an in-depth article about this one soon * Gastro intestinal - looking after our digestive system it’s super important because these disease are quite painful and will also affect our mental health. As a result this becomes even more importantIf you look at this list,We have some power over it. Some of these diseases are preventable with the right lifestyle which is eating whole food focused on nutrient density, eating enough fibre, working out and finding space to relax and decompress. Looking after your PCOS is not an option, it’s a mandatory action if we want quality of life as we age.Please note that this study was done based on medical codes. This means that they were inputted in a consultation with a healthcare professional so by default everyone had something. They did no look at PCOS women who have never come to a doctor’s office with a complain. In addition it doesn’t take in consideration lifestyle or dietary habits. I would treat the number with caution but take the lesson. The increased risk of disease for PCOS women has been replicated in numerous studies so it definetely exists. Ok, but we still have the question of does having PCOS affect how long we can live? Let’s go into some good news.The good newsA study published in 2023 followed a well-defined cohort of women diagnosed with PCOS, along with an age-matched reference group, for 32 years.Some key findings:No increase in all-cause mortality or CVD-related mortality was found in women with PCOS compared to the reference group, even at a mean age of 81 years.While women with PCOS showed a higher prevalence of CVD risk factors like hypertension and elevated triglycerides in earlier follow-ups (at perimenopausal age and mean age 71), these differences disappeared by the time they reached a mean age of 81.The only significant difference observed at baseline (32 years prior) between deceased and living women with PCOS was a higher waist-hip ratio (WHR) in the deceased group.This suggests that abdominal fat distribution might be a more critical factor in long-term health outcomes than previously thought.This is a bit confusing. We have higher risk of disease but doesn’t seem like it leads to us dying younger. The authors of this study proposed a few explanations of why:* The remaining higher testosterone levels in postmenopausal women with PCOS might have a protective effect, counteracting other CVD risk factors. We looked into what happens to women in Menopause in the article below.* The wedge resection surgery (no longer performed for us) that all the women with PCOS in this study underwent might have contributed to a reduction in PCOS symptoms and obesity, particularly abdominal obesity. However, the study does not definitively confirm whether the surgery itself is protective or not.The conflicting news3 other studies showed an increase in CVD risk for women with PCOS. The issue is that they don’t mention mortality but focus on incidence. However there is one abstract that is receiving a lot of attention from publications who showed a significantly higher mortality rate in women with PCOS. I am unable to find the whole study so I am only reporting on very little data on this study. I have emailed the journal for the full study.The researchers used ICD codes to identify 9,839 women with PCOS and matched them with 70,705 controls based on birth year and residential area from the Finnish Care Register for Health Care from 1969 to 2019. They then tracked mortality and causes of death. They found:Women with PCOS still had a 47% higher risk of dying during the study period compared to women without PCOSSome of the main causes:* Diabetes - a 207% higher risk of dying from diabetes compared to women without PCOS.* Other circulatory system diseases - 107% higher risk of dying from other circulatory system diseases compared to women without PCOS.* Bronchitis - 261% higher risk of dying from bronchitis compared to women without PCOS.* Tumors - 38% higher risk of dying from tumours compared to women without PCOS.The sadder part of this finding is that women with PCOS died younger than the control group (average age 51.4 years vs. 52.9 years).It’s important to note that the numbers of deaths were were 177 deaths/ 9839 for women with PCOS and 1,003/70,705. The sample size it’s small. We know there's a higher risk, but we don't know how many people actually died. The study doesn't tell us the incidence rates, which means we don't know how common these deaths actually were in both groups. It's like knowing it's more likely to rain tomorrow but not having a percentage chance.We don't know how long the researchers followed each person in the study. They collected data from 1969 to 2019, but people could have entered the study at any time. This makes it hard to compare the death rates accurately. Imagine comparing the number of car accidents on a busy road for a whole year versus just for one hour – it wouldn't be a fair comparison.Whilst this study might provoke a strong emotion, please bear in mind these are risk increases. It’s not an absolute terms that we will die at 50’s.Closing thoughtsTo conclude, yes, PCOS can affect how long we can live. Some of it will be in our control, some of it not quite. However, there is a powerful thing I am taking from writing this article and facing it: looking after ourselves is not negotiable. We can lead with emotions: it’s not fair, it’s annoying, it’s sad. Whilst we should allow ourselves to feel these emotions, our response is more important to it. I want to live till my ol
Hello everyone,Today we start discussing a super important topic: fertility.This will be a five part series to deep dive into our ability to conceive with my colleague Daria, a Nutritional Therapist who specialises in fertility. In these series we will answer some key questions about our fertility.* Episode 1: PCOS and fertility - how do I know how much time I have left?* Episode 2: How can I prepare my body for pregnancy?* Episode 3: The other side of the coin -> checking your partner’s fertility and optimising for a family* Episode 4: Finding ovulation when your cycles are irregular* Episode 5: The risk of miscarriageIt’s my birthday on Tuesday and I would love to give you a 20% discount on the paid version of The PCOS Newsletter. Available till 19th of February only. We have some incredible content coming up on top of our fertility series, including interviews with GPs and Gynaecologists. Don’t miss out on this offer. I know this is a worry for all of the women with PCOS. We hear about the probability of struggling to become pregnant from early on. It’s a worry for me. In addition to our struggles with fertility, there is also the annoying clock. Unfortunately finding the right husband it’s a bit trickier these days. If you have not found him at university or college, you are likely to be pushed with dating in your late twenties. By the time marriage comes along it will be early thirties. Unfortunately this age it’s also the time when your career picks up. You have enough experience to go up the ladder. With that comes access to more income which opens the doors to travelling and adventure. For me, the decision to have a baby now in my early thirties it’s though. I think I want to have children but I don’t want to give up my great life. Anyone feels the same?In today’s insightful conversation we discuss if and how you can find out your fertility status and why women with PCOS might struggle with fertility.In this article and video:* Who is Daria?* What is Nutritional Therapy in PCOS?* Why do women with PCOS struggle with fertility?* How do androgens impact fertility?* How do I know how much time I have left?* How does age impact fertility?* How long before planning should I prepare?* How do I know how much time he has got left?Who is Daria?Daria is Nutritional Therapist specialising in Fertility. She is a lecturer and academic tutor at CNM and a good friend of mine. You can find Daria at www.nutridaria.com, Instagram or email at: daria@nutridaria.comWhat is Nutritional Therapy in fertility?Nutritional therapists working in the realm of fertility prioritise two aims:* Getting the couple to optimal health * Replenish nutrients stores for a health babyRather than focusing solely on the woman, the approach emphasises that fertility is a shared journey, where both parties must be in optimal health. As a result we look at both the women and the man and address any imbalances. We leverage food and lifestyle as primary tools for health improvement. An essential aspect of the approach involves replenishing critical nutrients—such as iron, which plays a vital role in supporting the increased blood volume demands during pregnancy and preventing anemia. Addressing nutrient deficiencies prior to conception is crucial because correcting them during pregnancy can be significantly more challenging. Overall, the strategy is to prepare the couple holistically, reducing potential health risks and paving the way for a successful and healthy pregnancy journey.Why do women with PCOS struggle with fertility?Pregnancy can only happen when there is release of an egg from an ovary, a phenomenon called ovulation. There is a relatively small window of time around ovulation, called fertility window, when sperm has to be present in the female genitourinary tract for conception to occur. What can make it more challenging for women with PCOS to get pregnant is irregular ovulation patterns. Essentially we can’t predict when you should have intercourse in order for pregnancy to happen. It is important you understand why ovulation fails in women with PCOS to get the full picture of fertility. You can read it here:or watch it here:In addition to irregular periods, women with PCOS might have a lower quality eggs. Insulin resistance, a common feature of PCOS, can lead to oxidative stress, which damages eggs and impairs their developmental potential. Elevated androgen levels interfere with follicular development. It has also been shown that the follicular fluid in some women with PCOS shows a pro-inflammatory environment, increased oxidative stress, and metabolic disturbances which can adversely affect oocyte quality and preimplantation embryo development.Overall, some of the drivers of our PCOS symptoms doesn’t create the right type of environment for pregnancy. This is why working on our health is a non-negotiable if we want to have a baby.How do I know how much time I have left?If you come to your doctor and ask to assess how much time you have left to conceive they are most likely to perform testing of the ovation reserve.Your ovarian reserve refers to the quantity and quality of your remaining eggs. To measure your ovarian reserve, we have a few methods:* Anti-Müllerian Hormone (AMH): AMH is a hormone produced by granulosa cells in ovarian follicles and can be measured in a blood test. AMH level reflects the number of eggs that are present in the ovary and is therefore used to predict ovarian fertility potential and ovarian response to fertility drugs.* Antral Follicle Count (AFC): AFC refers to the number of small follicles (2-10 mm in diameter) visible on an ultrasound, typically measured early in the menstrual cycle, giving insight into your ovarian reserve.* Follicle-Stimulating Hormone (FSH): A basal (day 2–4) FSH concentration is an indirect marker of ovarian reserve based on feedback inhibition of pituitary FSH secretion. High FSH levels can indicate diminished ovarian reserve, but in PCOS, FSH is often normal or low.Women with PCOS often have elevated AMH levels and a higher antral follicle count (AFC) due to the high number of small and immature follicles, but this doesn’t always indicate good egg quality making it challenging to use AMH and AFC at a face value. Increased ovarian reserve markers like antral follicle counts and anti-Müllerian hormone levels in PCOS do not necessarily translate to a lengthened reproductive lifespan. It’s important to highlight that both AMH and AFC do not directly assess egg quality or the likelihood of successful pregnancy. Unfortunately, there is no direct method of measuring egg quality at the moment.Overall, it challenging to know how much time you have left for any women. It is even more challenging for us, those with PCOS. If your PCOS is relatively controlled and its severity mild, the above methodologies could give you an indication of where you are standing with your PCOS. How does age impact fertility?Oocyte number and quality decline with age; however, fertility varies significantly even among women of the same age. In general fertility starts to decline in women of 30 years of age with an accelerated decline starting around 35-37 years with a more pronounced effect >40 years.While PCOS doesn’t directly accelerate the natural decline in egg quality with age, time remains a critical factor. Whilst some research suggests women with PCOS could retain their ovarian reserve longer than those without the condition, other data show that women with PCOS face similar age-related declines in fertility.How long before planning should I prepare?The earlier you start, the better. Ideally, aim to begin preparation at least 3 to 6 months before trying to conceive. This time frame gives your eggs the chance to mature in an optimal environment. It takes 3 months for a follicle to develop so we want to give it the best chance. If you have less time, don’t worry as any amount of preparation is beneficial. We will delve deeper into this topic in our next episode.How do I know how much time he has got left?It’s a 50% 50% job to make a baby. Even though we do much more of the work of actually delivery the baby, for its conception we need the sperm health to be as good as our health. For man, fertility also declines with age, even though not as rapid as ours. To understand your partner’s fertility:* Semen analysis - this involves a sample of your partner’s semen being tested to check the amount of sperm in it. The test also checks how fast the sperm move and the shape of the sperm.* Semen DNA fragmentation - The human sperm cell, in fact, is not just responsible for the expression of the father’s genes but also for activation and the development of the embryo during and after implantation. This test checks for any problems in the DNA material. We will also delve deeper into this topic in Episode 3.I hope this has allowed you to get a little insight into why fertility might be challenging for us. See you next Sunday,Francesca This is a public episode. If you'd like to discuss this with other subscribers or get access to bonus episodes, visit www.thepcosnewsletter.com/subscribe